How Physiotherapy Helps Mobility Improvement
A Doctor’s Practical Guide for Patients and Caregivers
Physiotherapy is often misunderstood as “exercise therapy” or something you try only after pain becomes unbearable. In real clinical practice, it is much broader and far more precise than that.
As a physiotherapy doctor treating musculoskeletal pain, neurological conditions, balance disorders, post-surgical cases, and chronic pain daily, I see two types of patients:
- Those who come early, recover faster, and avoid complications
- Those who come late, after months of wrong treatment, rest, or internet advice
This article is written to help you be in the first group.
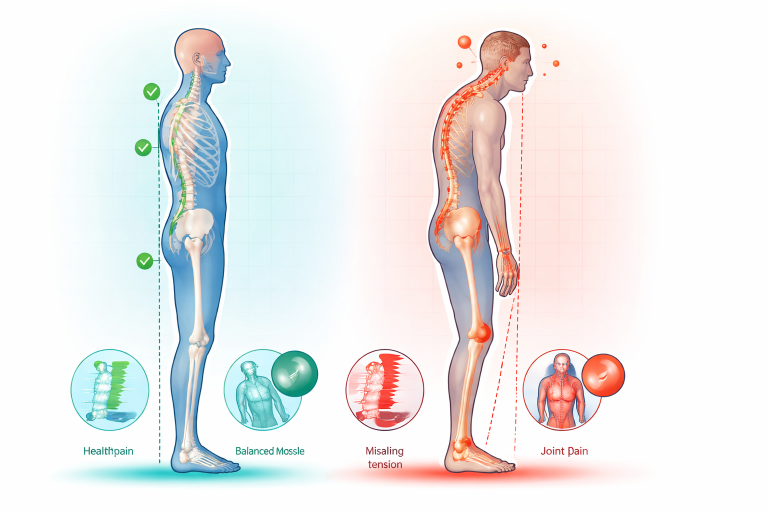
What Physiotherapy Actually Treats (Beyond Pain Relief)
Physiotherapy focuses on restoring movement, control, strength, balance, and function — not just reducing pain temporarily. Understanding how targeted therapy restores movement helps patients see why personalized treatment plans are designed to improve long-term mobility rather than just provide short-term relief.
Pain is often a symptom. The real problem may be:
Pain usually signals an underlying issue rather than being the actual cause. Movement faults, weakness, stiffness, or nerve involvement often create ongoing stress in the body. Identifying the root problem is essential for lasting recovery.
Poor movement patterns
When the body moves incorrectly due to habit, weakness, or past injury, certain areas get overloaded. Over time, this leads to pain and reduced function. Correcting movement patterns prevents repeated strain.
Muscle imbalance
- “Physiotherapy fixes everything in 10 sessions”
- “One exercise fits all back pain”
- “Vertigo is only a neck problem”
- “Parkinson’s can’t improve with physiotherapy” (this is flat-out wrong)
My honest observation
Some muscles become tight and overactive while others remain weak. This imbalance alters joint mechanics and increases pain during daily activities. Balanced strengthening helps restore proper movement control, which is a key principle in advanced physiotherapy for mobility issues.
Joint stiffness or instability
Stiff joints restrict movement, while unstable joints lack proper control. Both conditions place abnormal stress on surrounding tissues. Physiotherapy restores safe mobility and joint stability.
Nerve involvement
Nerve-related pain often presents as tingling, burning, or radiating symptoms. It usually results from irritation or compression rather than muscle damage. Proper assessment is crucial for safe treatment.
Loss of coordination after neurological damage
Neurological damage can disrupt coordination even when strength is present. This leads to inefficient movement and higher injury risk. Physiotherapy retrains control and functional movement safely. Treating only pain without addressing the cause is why many patients relapse.
Step 1: Check Specialization, Not Just Degree
Poor balance or frequent falls
Balance problems often occur when the brain and muscles fail to coordinate properly. This increases the risk of falls and injuries during daily activities. Physiotherapy focuses on balance retraining and safe movement strategies.
Muscle stiffness or weakness
Stiff or weak muscles limit smooth and controlled movement. This can make simple tasks feel exhausting or painful. Targeted therapy helps restore flexibility, strength, and functional use.
Difficulty walking, standing, or using hands
Problems with walking, standing, or hand function usually indicate impaired coordination or strength. These limitations affect independence and daily life. Physiotherapy works on task-specific training to regain function.
Loss of confidence in daily activities
Repeated difficulty or fear of falling often reduces confidence. Patients may avoid movement, which worsens the condition. Guided rehabilitation helps rebuild trust in the body and safe independence.
What Physiotherapy Does Here
Neurological physiotherapy is not about general fitness or gym workouts. It focuses on retraining the nervous system to control movement safely and efficiently. Treatment is structured, goal-based, and tailored to daily functional needs.
Loss of confidence in daily activities
After neurological injury, the body often adopts faulty movement patterns. Physiotherapy helps correct these patterns through guided, repetitive practice. This improves efficiency and reduces strain during daily activities.
Improving balance reactions
Neurological conditions can slow or disrupt balance responses. Therapy trains the body to react appropriately to changes in position. This significantly reduces the risk of falls.
Teaching the brain to re-learn tasks
The brain has the ability to adapt and relearn through repetition and feedback. Physiotherapy uses task-specific training to rebuild lost skills. This supports functional recovery over time.
Preventing stiffness and deformity
Reduced movement can lead to muscle tightness and joint deformities. Early and consistent physiotherapy maintains flexibility and joint health. This prevents long-term complications and disability.
Real Clinical Insight
A stroke patient may regain muscle strength but still struggle to walk safely because balance and coordination were never retrained. Strength alone is not recovery.
Who Benefits Most
Early-stage stroke patients
Patients who start physiotherapy early after a stroke recover movement and balance more effectively. Early intervention prevents stiffness, weakness, and unsafe movement habits. This improves long-term independence.
Parkinson’s patients with freezing or instability
Physiotherapy helps manage freezing episodes and balance problems common in Parkinson’s disease. Targeted training improves gait control and reduces fall risk. This allows safer daily mobility.
MS patients aiming to preserve independence
Multiple sclerosis can gradually affect strength, balance, and coordination. Physiotherapy focuses on energy-efficient movement and symptom management. This helps patients maintain function and independence for longer.
When Physiotherapy Is Not Enough
If symptoms worsen rapidly, cognition declines, or new weakness appears, neurological evaluation and imaging are essential before continuing therapy.
2. Breathing & Respiratory Physiotherapy
Breathing problems are often treated only with medication, but lungs also need mechanical training.
What Respiratory Physiotherapy Includes
Breathing control techniques
These techniques teach patients how to breathe more efficiently rather than more forcefully. Controlled breathing reduces breathlessness and anxiety. It also improves oxygen use during daily activities.
Chest expansion exercises
Chest expansion exercises improve rib and lung movement. They help increase lung capacity and prevent stiffness of the chest wall. This supports easier and deeper breathing.
Airway clearance methods
These methods help loosen and clear mucus from the lungs. They are especially useful for chronic respiratory conditions. Clearing airways reduces infections and breathing difficulty.
Postural correction to improve lung capacity
Poor posture restricts chest movement and lung expansion. Postural correction allows the lungs to expand fully. This improves breathing efficiency and reduces fatigue.
Common Patient Mistake
Many patients “breathe more” instead of “breathe better,” which increases fatigue and anxiety.
Clinical Reality
Respiratory physiotherapy reduces hospital admissions, but it works best when started before severe breathlessness develops.
3. Sports & Activity-Related Physiotherapy
Physiotherapy is not only for injured athletes — it’s for preventing injuries before they happen.
What It Corrects
Poor movement mechanics
Incorrect movement mechanics place unnecessary stress on muscles and joints. Over time, this leads to pain and repeated injuries. Physiotherapy corrects how the body moves during daily and sports activities.
Muscle dominance and weakness patterns
When certain muscles overwork while others remain weak, movement becomes inefficient. This imbalance increases injury risk and limits performance. Targeted training restores balanced muscle function.
Joint overload due to faulty technique
Poor technique during exercise or work overloads specific joints. This causes inflammation, pain, and reduced performance. Physiotherapy refines technique to protect joints and improve efficiency.
Example from Practice
A runner with repeated knee pain often doesn’t have a knee problem — the issue is usually hip control or ankle mobility.
What Doesn’t Work
Rest without correction
Prolonged rest may reduce pain temporarily but does not fix the underlying problem. Without correcting movement or weakness, pain often returns. This approach can delay proper recovery.
Painkillers without movement assessment
Pain medication can mask symptoms without addressing the cause. Continuing faulty movement while pain is suppressed increases the risk of long-term damage. Assessment is essential before treatment.
Random online exercise programs
Generic exercises ignore individual limitations and diagnosis. The wrong exercises can worsen pain or cause new injuries. Rehabilitation must be personalized to be safe and effective.
4. Posture, Lifestyle & Work-Related Pain
Poor posture is rarely the root cause — it’s usually a result of muscle imbalance and fatigue.
Strengthening underused muscles
Weak or inactive muscles fail to support joints properly. This leads to overload and pain in other areas. Targeted strengthening restores balance and reduces strain.
Improving joint mobility
Restricted joints force the body to compensate with poor movement. This increases stress on surrounding tissues. Improving mobility allows smoother, pain-free movement.
Teaching sustainable work and sleep habits
Poor work posture and sleep positions repeatedly stress the body. Small daily habits often maintain pain without patients realizing it. Physiotherapy educates on practical changes that support long-term recovery.
Important Truth
“Sit straight” advice alone does not fix posture. Your body returns to bad posture when it lacks strength or endurance.
5. Joint Pain, Stiffness & Arthritis Management
Joint pain may come from:
Inflammation
Inflammation in a joint causes pain, swelling, and reduced movement. Physiotherapy helps manage symptoms while supporting healing through gentle exercises and movement.
Degeneration
Joint degeneration, such as in osteoarthritis, gradually reduces cartilage and mobility. Targeted therapy maintains function, reduces strain, and slows progression.
Muscle weakness
Weak muscles fail to support joints properly, increasing pain and injury risk. Strengthening exercises restore support and improve daily function.
Poor joint alignment
Misaligned joints alter movement patterns and load distribution. Physiotherapy corrects alignment through exercises and manual techniques to reduce stress and prevent further damage.
Physiotherapy Helps By
Reducing joint stress
Physiotherapy teaches proper movement and load distribution to protect painful or vulnerable joints. This reduces wear and prevents further injury.
Improving surrounding muscle support
Strengthening the muscles around a joint stabilizes it and absorbs stress. This improves function and decreases pain during daily activities.
Maintaining mobility and independence
Regular therapy keeps joints flexible and muscles strong, allowing patients to perform daily tasks safely. It helps preserve independence and quality of life.
Who Should Be Careful
Sudden inability to bear weight
These require medical evaluation before therapy.

What a Proper Physiotherapy Plan Looks Like
Step 1: Detailed Assessment
Movement analysis
Examine how you move to identify faulty patterns that cause pain or injury.
Strength testing
Measures muscle power to identify weak areas that may limit movement or joint support. It helps guide safe, targeted exercises.
Functional limitations
Assesses which daily activities are difficult due to pain, weakness, or mobility issues. This guides therapy toward real-life improvements.
Red flag screening
Checks for warning signs like severe pain, sudden weakness, or neurological deficits. Detecting these early ensures urgent medical attention if needed.
Step 2: Clear Diagnosis Explanation
You should understand:
What structure is involved
Identifying the specific muscle, joint, or nerve causing pain is essential. This helps tailor treatment to the root problem rather than just addressing symptoms.
Why pain started
Understanding the cause—whether injury, overuse, posture, or neurological issue—guides effective therapy. It prevents recurrence by addressing the underlying reason.
What activities worsen or help it
Knowing which movements or habits aggravate or relieve pain helps patients modify daily activities safely. This ensures faster recovery and reduces the risk of flare-ups.
Step 3: Individualized Treatment
No “same exercises for everyone.”
Step 4: Home Guidance
Correct dosage matters more than exercise count.
Step 5: Reassessment & Progress Tracking
If progress is unclear, the plan must change.
Step 4: Evaluate Therapist Involvement
Correct dosage matters more than exercise count.
Step 5: Reassessment & Progress Tracking
If progress is unclear, the plan must change.

Common Myths Patients Believe (And Why They’re Harmful)
- “Pain means rest completely”
- “Physiotherapy is only massage”
- “Exercises are the same for everyone”
- “If it hurts, it’s working”
These beliefs delay recovery and worsen chronic pain.
Therapist-guided sessions

How Long Does Recovery Really Take?
Acute muscle or joint issues: 2–6 weeks
Simple strains or sprains often improve within a few weeks with guided therapy. Early intervention speeds healing and prevents complications.
Minimal over-dependence on machines
Post-surgical rehab: 6–12 weeks or more
Recovery after surgery requires structured exercises to restore strength, mobility, and function. Progress depends on the type of surgery and patient adherence.
Neurological conditions: long-term, phased recovery
Stroke, Parkinson’s, or MS patients may need months of gradual, goal-based therapy. Recovery focuses on regaining safe, functional movement over time.
Quick fixes are rare. Safe recovery is progressive and monitored.
Lasting improvement requires consistent, monitored therapy. Sudden or unsupervised changes can delay recovery or cause setbacks.
Read More:- Best Posture For Reducing Lower Back Pain
Conclusion:
Physiotherapy works best when it is:
- Started early
- Properly assessed
- Individually planned
- Regularly reassessed
It is not a last resort — it is a clinical tool for restoring quality of life when used correctly.
If you want, I can next:
- Rewrite this for Vertigo, Parkinson’s, Stroke, or Sciatica
- Adapt it for a clinic website or Google Business Profile
- Convert it into patient FAQs or short explainer posts
Physiotherapy Clinic in ahmedabad - FAQs
Q1. Is physiotherapy only for people in pain?
Q2. How long does physiotherapy take to show results?
Q3. Will physiotherapy exercises hurt?
Q4. Can physiotherapy replace surgery or medication?
Q5. How often should I attend physiotherapy sessions?
References
About the Author

Dr. Hetal M Varia
After a rich experience of working in US healthcare as manager and licensed physiotherapist in US for last 11 years, she has returned home with a vision to become pioneer of Vestibular Therapy and specialized Parkinson physiotherapy in Ahmedabad. With her special skills and expertise in vertigo, Parkinson, balance and movement disorders therapy, Dr. Varia is committed to provide US standards of therapy services , compassionate and patient centered care to our people and community. With a vision of the world where everyone walks strong & steady, she intends to empower individuals with vestibular and neurological disorders through specialized care, rehabilitation & innovative therapies to improve mobility, balance & overall quality of life!