Best Posture For Reducing Lower Back Pain
In my daily physiotherapy practice, posture alone is rarely the sole cause of lower back pain and fixing posture alone is rarely the full solution. However, poor or sustained postures can overload the spine, delay healing, and repeatedly trigger pain even after treatment.
This article will help you understand:
- What “good posture” really means for your back
- Which postures reduce pain — and which quietly worsen it
- What to correct first, what to ignore, and when posture work is not enough
I’m writing this exactly how I explain it to patients in the clinic — clearly, safely, and without false promises.
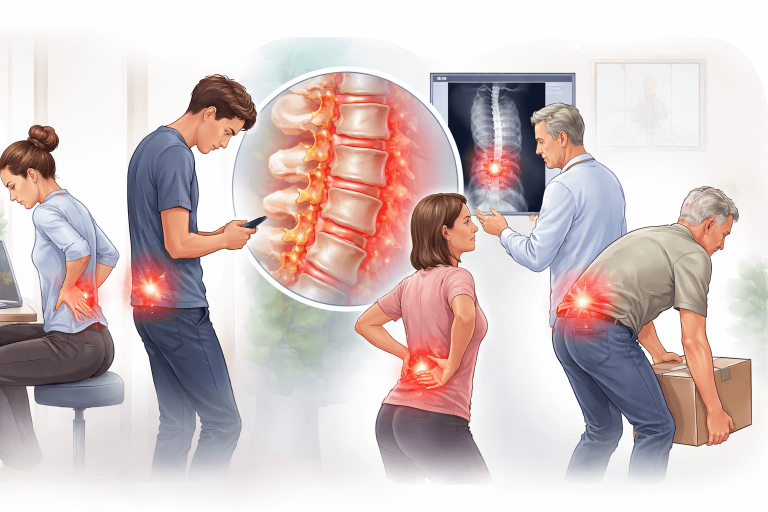
Why posture affects lower back pain (in real patients, not diagrams)
Your lower back (lumbar spine) is designed for movement, not for staying still in one “perfect” position.
When posture contributes to pain, it usually does so by:
Sustained spinal loading (long sitting, standing, phone use)
Holding the spine in one position for long periods increases pressure on discs and joints, leading to discomfort and pain over time.
Muscle fatigue rather than muscle weakness
Back pain often arises from tired muscles that can’t support the spine, not weak muscles. Frequent movement helps reduce fatigue.
Reduced blood flow to spinal tissues
Prolonged static positions limit circulation, slowing nutrient delivery and tissue recovery, which can worsen stiffness and pain.
Repeated micro-strain on discs and facet joints
Small, repeated stresses from poor posture accumulate over time, irritating spinal structures and increasing the risk of chronic pain.
Common posture myths I correct every day
Myth 1: “Sit straight at all times.”
Forcing an upright posture increases muscle tension and fatigue.
Myth 2: “Bad posture causes slipped discs.”
Disc problems are multifactorial posture alone is rarely the cause.
Myth 3: “Correct posture will cure back pain.”
Posture supports recovery; it does not replace diagnosis or treatment.
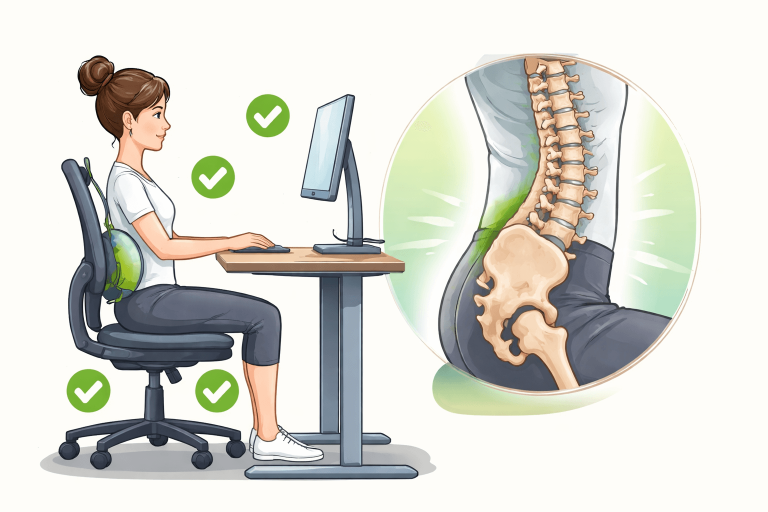
Best sitting posture for lower back pain (clinically practical)
What actually helps
Sit with natural lumbar curve, not exaggerated arching
Maintain your back’s natural inward curve without forcing it, as over-arching increases muscle fatigue. A relaxed, supported curve reduces strain on spinal joints.
Feet flat on the floor
Keeping feet supported helps balance the pelvis and reduces lower back load. Use a footrest if your feet don’t reach the floor comfortably.
Hips slightly higher than knees
This position reduces disc pressure and helps prevent slouching. Small seat-height adjustments can significantly ease lower back strain.
Back supported — chair or lumbar roll
Back support reduces continuous muscle effort during sitting. A chair back or lumbar roll helps prevent pain from prolonged sitting.
Screen at eye level to avoid slouching
An eye-level screen prevents forward head posture and spinal overload. This simple change reduces neck and lower back stress during work.
What I tell desk-job patients
“Your posture should feel supported and relaxed, not forced.”
Most important rule:
Change position every 30–40 minutes, even if posture is “perfect”.
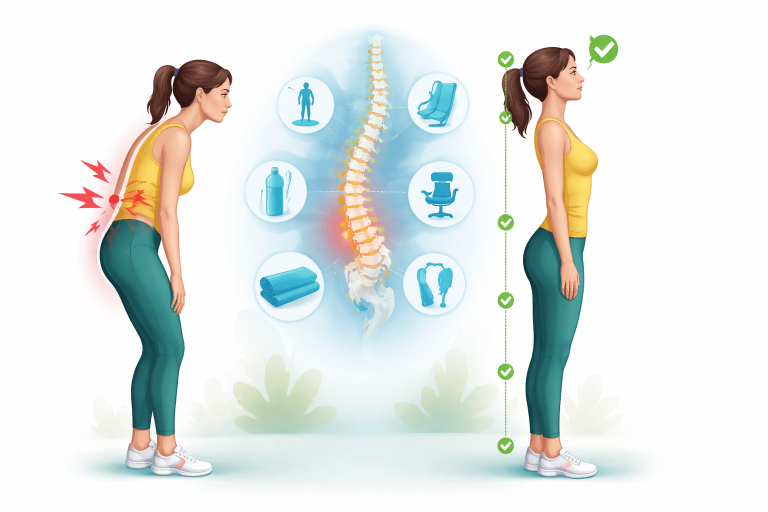
Best standing posture for back pain
When standing for long periods:
Distribute weight evenly on both feet
Stand with weight balanced to reduce strain on your lower back and hips. Uneven weight shifts can overload one side, causing fatigue and pain.
Avoid locking knees
Keep knees slightly bent to maintain natural spinal alignment and prevent joint stress. Locked knees increase tension in the lower back and legs, so maintaining a correct posture for lower back pain relief is essential for reducing strain and supporting spinal health.
Gently engage core (no bracing)
Activate abdominal muscles lightly to support your spine without stiffening your body. Over-bracing can cause tension and restrict natural movement.
Shift weight occasionally
Change stance or move slightly every few minutes to prevent muscle fatigue and improve blood circulation. Staying still increases spinal load and discomfort.
Use a small footrest if standing for work (alternate legs)
Elevating one foot occasionally reduces lower back strain and promotes a relaxed posture. Alternate legs to balance spinal load and prevent stiffness.
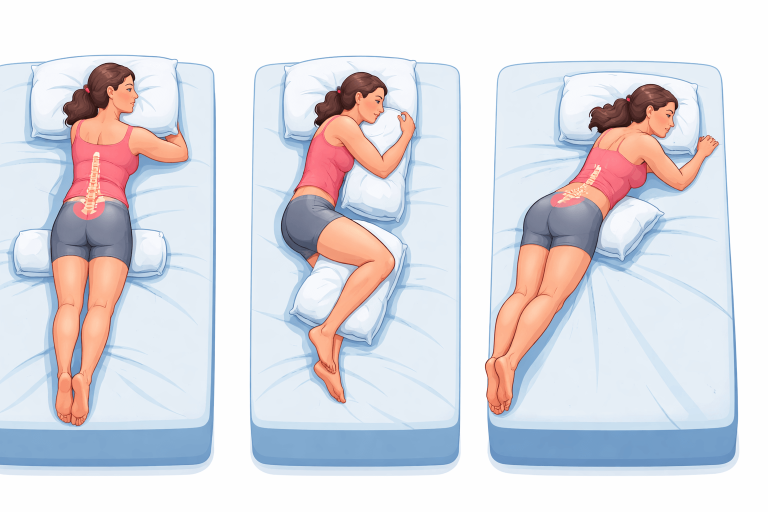
Best sleeping posture for lower back pain
Side sleeping (most patients)
- Pillow between knees
- Neck aligned with spine
- Avoid curling too tight
Back sleeping
- Pillow under knees
- Medium-firm mattress
- Avoid high pillows under head
What to avoid
- Sleeping on stomach (common pain trigger)
- Very soft or sagging mattress

Postures that silently worsen back pain
From real patient patterns:
- Sitting on bed or sofa without back support
- Phone use with bent neck + rounded back
- Long driving without lumbar support
- One-sided sitting (wallet, crossed legs)
Step-by-step: What patients should do first, next, and later
Step 1: Rule out serious causes
If pain includes:
Leg numbness or weakness
This may indicate nerve involvement or serious spinal issues. Immediate medical evaluation is needed rather than just posture correction.
Night pain not relieved by rest
Persistent pain at night can signal an underlying condition beyond muscle strain, requiring professional assessment.
Sudden bowel/bladder issues
Loss of control or changes in bowel/bladder function can indicate a medical emergency like cauda equina syndrome. Seek urgent medical care.
Fever or unexplained weight loss
These may suggest infection, inflammation, or systemic illness. Do not ignore — see a doctor promptly for proper diagnosis.
Step 2: Reduce overload (before exercises)
- Modify sitting time
- Improve sleep posture
- Adjust workstation
- Stop painful activities temporarily
Pain reduction comes before strengthening.
Step 3: Start targeted physiotherapy
Posture correction works best when combined with:
Core endurance training
Strengthens deep abdominal and back muscles to support the spine during daily activities. Improves stability and reduces the risk of recurring lower back pain.
Hip mobility work
Increases flexibility in the hips, which helps the lower back move naturally and reduces compensatory strain. Essential for safe bending, lifting, and walking.
Load-management education
Teaches how to lift, carry, and sit safely to avoid overloading the spine. Helps patients prevent flare-ups and maintain long-term back health.
Breathing and movement retraining
Promotes proper breathing patterns that support spinal stability and reduces unnecessary tension. Helps coordinate safe, efficient movement during daily tasks.

Real clinical case (anonymized)
Patient: 34-year-old IT professional
Complaint: Chronic lower back pain for 8 months
Tried: Posture belts, ergonomic chair, YouTube posture drills
Problem:
Sat “upright” for 6–7 hours
Sitting rigidly for long periods increases muscle fatigue and spinal strain. Even a “perfect” posture can cause pain if movement is lacking.
Over-braced core muscles
Tensing abdominal muscles too much restricts natural movement and increases discomfort. A relaxed, supportive engagement is more effective.
No movement variability
Staying in one position overloads spinal joints and muscles. Regular micro-movements or position changes are essential to prevent pain.
Treatment focus:
Movement breaks
Short, frequent breaks reduce spinal load and restore circulation, helping muscles recover during prolonged sitting.
Relaxed sitting posture
Supporting the natural curve of the spine without forcing it prevents unnecessary tension and discomfort.
Gradual spinal loading exercises
Progressive exercises strengthen spinal and core muscles safely, improving endurance and reducing the risk of recurrent back pain.
Outcome:
Pain reduced within 3 weeks, returned to work comfortably in 6 weeks.

When posture correction is NOT enough
Posture alone won’t resolve pain if you have:
Disc bulge with nerve involvement
A bulging disc pressing on nerves can cause pain, numbness, or weakness in the legs. Posture correction alone is insufficient; targeted physiotherapy is needed.
Facet joint arthritis
Arthritic changes in the small spinal joints can cause localized back pain and stiffness. Management requires guided exercises and load modification.
Spondylolisthesis
A condition where one vertebra slips over another, leading to instability and pain. Safe movement, core strengthening, and professional supervision are essential.
Post-surgical stiffness
After spine surgery, tissues can become tight and weak. Gradual physiotherapy restores mobility, strength, and functional posture.
Chronic pain sensitization
Long-standing pain can make the nervous system more sensitive, causing discomfort even with minor movements. Treatment includes graded exercise, education, and pain management strategies.

Home mistakes that delay recovery
I see these daily:
- Wearing posture correctors all day
- Copying random exercises from social media
- Avoiding all activity out of fear
- Ignoring early pain signals
- Expecting instant relief

How long does improvement realistically take?
For most uncomplicated mechanical back pain:
- Initial relief: 1–2 weeks
- Functional improvement: 4–6 weeks
- Long-term control: 8–12 weeks
CONCLUSION
Good posture is:
- Dynamic, not rigid
- Supportive, not forced
- Combined with movement and strength
If you remember only one thing: The best posture is the next posture.
If your back pain keeps returning despite posture correction, don’t self-blame it usually means the problem hasn’t been properly assessed yet.
Best Posture For Reducing Lower Back Pain: FAQs
Q1. Is there one “perfect posture” that prevents lower back pain?
Q2. Do posture corrector belts actually help lower back pain?
Q3. How long should I sit before changing my posture or taking a break?
Q4. Can poor posture cause disc bulge or slipped disc?
Q5. When should I see a physiotherapist instead of just fixing posture at home?
References
About the Author

Dr. Hetal M Varia
After a rich experience of working in US healthcare as manager and licensed physiotherapist in US for last 11 years, she has returned home with a vision to become pioneer of Vestibular Therapy and specialized Parkinson physiotherapy in Ahmedabad. With her special skills and expertise in vertigo, Parkinson, balance and movement disorders therapy, Dr. Varia is committed to provide US standards of therapy services , compassionate and patient centered care to our people and community. With a vision of the world where everyone walks strong & steady, she intends to empower individuals with vestibular and neurological disorders through specialized care, rehabilitation & innovative therapies to improve mobility, balance & overall quality of life!