Gradual balance retraining helped restore postural control and confidence over three weeks. The patient resumed daily activities without fear of dizziness or instability.
Vestibular Rehabilitation Therapy: Step-By-Step Guide
Feeling dizzy, off-balance, or as if the room is spinning can be frightening.
Many patients I see say the same thing in the clinic:
Doctor, I’m scared to move my head.
I don’t trust my balance anymore.
Everyone says it’s anxiety, but it doesn’t feel like that.
Vestibular therapy exists precisely for these patients — but only when used correctly, for the right diagnosis, and at the right time.
This guide explains what vestibular therapy really is, who benefits, what it can and cannot fix, and how to approach treatment safely and realistically.

What Is Vestibular Therapy — In Simple Terms?
Vestibular therapy is a specialized branch of physiotherapy designed to help people whose dizziness or balance problems come from faulty communication between the inner ear, eyes, neck, and brain.
It is not a general exercise.
It is not yoga.
It is not random head movements from YouTube.
It is a targeted neurological retraining process that helps the brain adapt, recalibrate, or compensate when balance signals are disturbed.
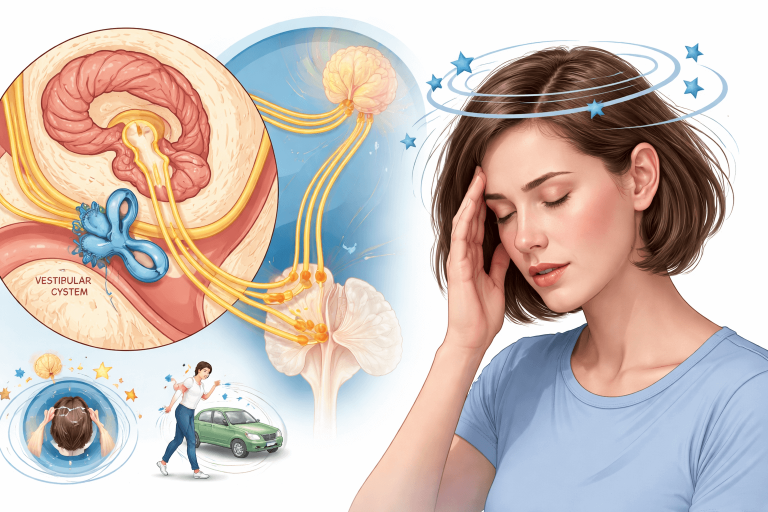
Understanding the Vestibular System (Why Dizziness Happens)
Your sense of balance comes from three systems working together:
1. Inner ear (vestibular system) – detects head movement and position
The inner ear senses head motion, speed, and direction, sending real-time signals to the brain. When this system is disturbed, the brain receives incorrect movement information, leading to vertigo, dizziness, or imbalance.
2. Eyes (visual system) – tells you where you are in space
The visual system provides constant feedback about your body’s position and movement in the environment. If eye–brain coordination is affected, patients may feel dizzy, disoriented, or unstable, especially during head or body movement.
3. Muscles & joints (proprioception) – especially neck and legs
Proprioception comes from muscles and joints, helping the brain sense body position without looking. Poor neck mobility, weak legs, or joint stiffness can distort these signals and contribute to unsteadiness or balance loss.
The brain constantly cross-checks all three.
When one system sends incorrect or delayed signals, the brain gets confused — and you may experience:
Spinning sensation (vertigo)
Vertigo feels like the room or your body is rotating, often triggered by head movements or position changes. It usually indicates a problem in the inner ear or its connection with the brain.
Light-headedness or floating
This sensation is described as feeling faint, woozy, or disconnected from the ground. It may worsen with standing, walking, or quick movements and is commonly linked to balance system mismatch.
Nausea
Nausea occurs when the brain receives conflicting signals from the inner ear, eyes, and body. This sensory confusion often accompanies vertigo and may increase with movement.
Blurred vision when moving the head
Blurred or jumping vision during head movement suggests poor eye–head coordination. Patients may find it difficult to read signs or focus while walking or turning.
Unsteady walking or fear of falling
Balance instability can make walking feel unsafe, especially on uneven surfaces or in crowds. Over time, fear of falling may lead patients to restrict movement, which can worsen balance further.
Vestibular therapy helps the brain re-learn how to trust and integrate these signals again.
Common Conditions That Truly Benefit from Vestibular Therapy
In real clinical practice, vestibular rehabilitation works best for specific diagnoses, not “all dizziness.”
Benign Paroxysmal Positional Vertigo (BPPV)
BPPV is one of the most common causes of vertigo and occurs due to a mechanical problem inside the inner ear. It typically causes brief but intense dizziness with specific head movements.
Sudden spinning with head movements
Patients experience brief episodes of spinning when turning in bed, looking up, or bending forward. Symptoms are positional and stop when the head is kept still.
Caused by displaced calcium crystals in the inner ear
Tiny calcium particles move into the wrong part of the inner ear, sending false movement signals to the brain. This mismatch triggers sudden vertigo.
Often improves dramatically within 1–3 sessions when treated correctly
When accurately diagnosed, specific repositioning maneuvers can relieve symptoms quickly. Random exercises or delays in treatment may prolong recovery.
Vestibular Neuritis / Labyrinthitis
These conditions involve inflammation of the inner ear, usually following a viral infection. Symptoms are more constant and disabling than BPPV.
Post-viral inner ear inflammation
The vestibular nerve or inner ear structures become inflamed after a viral illness. This disrupts balance signals and causes persistent dizziness.
Severe dizziness initially, followed by lingering imbalance
Patients often report sudden, intense vertigo that gradually settles, leaving behind unsteadiness. Quick head movements may remain uncomfortable for weeks.
Therapy focuses on brain compensation and movement tolerance
Physiotherapy helps the brain adapt to the damaged balance input. Gradual, controlled movements are used to restore confidence and stability.
Post-Concussion Dizziness
Dizziness after a head injury is common and often multifactorial. It may involve the inner ear, vision, neck, and brain processing together.
Common after head injury or whiplash
Even mild concussions or sudden neck movements can disrupt balance systems. Symptoms may appear immediately or days after the injury.
Often involves eye movement and balance coordination issues
Patients may struggle with focusing, reading, or walking in busy environments. These problems come from poor coordination between vision and balance systems.
Requires careful progression — not aggressive exercises
Overloading the system too early can worsen symptoms. A slow, graded rehabilitation approach is essential for safe and effective recovery.
Vestibular Migraine
Vestibular migraine is a neurological condition where dizziness is a dominant symptom, sometimes occurring even without a typical migraine headache. Symptoms can vary in intensity and frequency.
Dizziness with or without headache
Patients may experience vertigo, imbalance, or motion sensitivity even when head pain is absent. This often leads to confusion and delayed diagnosis.
Trigger-based, fluctuating symptoms
Episodes may be triggered by stress, lack of sleep, certain foods, or visual overload. Symptoms tend to come and go rather than remain constant.
Therapy helps improve stability between episodes (not a cure for migraine itself)
Physiotherapy focuses on balance control, visual stability, and movement confidence. It supports daily function but does not replace medical migraine management.
Cervicogenic (Neck-Related) Dizziness
Cervicogenic dizziness arises from dysfunction in the neck rather than the inner ear. It is commonly associated with posture problems or neck injury.
Dizziness linked to neck stiffness, posture, or injury
Poor neck mobility or sustained poor posture can alter balance signals to the brain. Dizziness often worsens with neck movement or prolonged positions.
Requires combined neck + vestibular treatment
Treatment must address both neck mechanics and balance retraining. Treating only one component often leads to incomplete recovery.
Often missed or misdiagnosed
Because scans are usually normal, this condition is frequently mistaken for anxiety or inner ear disorders. Careful clinical assessment is essential for accurate diagnosis.

Conditions Commonly Mismanaged With Vestibular Therapy
As a clinician, I must be honest — vestibular therapy is not a solution for everything.
It is NOT effective alone for:
Vestibular physiotherapy has clear limitations and should not be used as a standalone treatment in certain conditions, which is why step-by-step vestibular rehab at Ahmedabad physiotherapy clinic should be guided carefully and integrated with appropriate medical care. Identifying these situations early helps prevent delays in proper medical care.
Active Meniere’s disease flare-ups
During acute episodes, vertigo is driven by inner ear fluid imbalance. Medical management is required first, with physiotherapy playing a supportive role only between attacks.
Severe uncontrolled anxiety or panic disorders
Dizziness here is often driven by the nervous system rather than balanced organs. Psychological and medical treatment must be addressed before vestibular exercises can help.
Cardiac-related dizziness
Dizziness caused by heart rhythm or blood flow issues requires urgent medical evaluation. Physiotherapy does not address the underlying cardiovascular cause.
Low blood pressure–related fainting
Symptoms related to sudden drops in blood pressure need medical investigation and lifestyle or medication adjustment. Balance exercises alone will not prevent fainting episodes.
Brain tumors or stroke-related dizziness (without medical clearance)
Central nervous system causes of dizziness must be ruled out or medically stabilized first. Vestibular therapy should begin only after specialist clearance and diagnosis.
This is why proper diagnosis always comes before exercises.

What Vestibular Therapy Actually Involves (Clinically)
1. Gaze Stabilization Training
Gaze stabilization exercises improve the coordination between eye and head movements. They are designed to restore visual clarity and reduce dizziness during everyday activities.
Blurred vision during head movement
Patients may feel objects shift or blur when the head moves. These exercises train the eyes to stay focused while the head is in motion.
Dizziness while walking or turning
Poor eye–head control can cause dizziness during walking or direction changes. Training emphasizes controlled movement rather than speed.
2. Balance Retraining
Balance retraining helps rebuild stability and confidence in standing and walking. Progression is gradual and based on safety and individual ability.
Progresses from:
Static standing → dynamic movement → real-life walking tasks
Exercises begin with simple standing balance and advance to walking, turning, and functional tasks. Each stage prepares the body for real-world movement.
3. Habituation (Only When Appropriate)
Habituation involves carefully controlled exposure to movements that trigger dizziness. It is used selectively, depending on diagnosis and symptom response.
This approach helps reduce movement sensitivity and improve tolerance over time. Exercises must be precisely dosed, as overexposure can worsen symptoms.
Controlled exposure to symptom-provoking movements to:
- Reduce sensitivity
- Improve tolerance
This must be dosed carefully — more is not better.
4. Neck & Postural Treatment (Often Ignored)
Neck dysfunction and poor posture can significantly contribute to dizziness and balance problems. Addressing these factors is essential for lasting recovery.
Especially important in:
Desk workers
Prolonged sitting and forward head posture can strain the neck and alter balance input. Postural correction and mobility exercises are key.
Whiplash patients
Neck injuries can disrupt proprioceptive signals, leading to dizziness. Treatment combines gentle neck rehabilitation with vestibular care.
Cervicogenic dizziness
When dizziness originates from the neck, isolated vestibular exercises are insufficient. A combined neck and balance approach gives better outcomes.
Ignoring the neck is a common reason therapy fails.

Doctor, I Feel Worse After Exercises — Is That Normal?
A mild, temporary increase in symptoms can be normal, especially early on.
However:
Symptoms should settle within minutes to hours
Mild dizziness after exercises is expected early in therapy, but it should calm down within a short time. Persistent or prolonged symptoms suggest the exercises may need adjustment.
Dizziness should not escalate session after session
Each session should feel similar or slightly easier than the previous one. Worsening dizziness over multiple sessions is a sign that progression is too fast.
Severe nausea, headaches, or imbalance mean the program is too aggressive
Strong nausea, intense headaches, or increased unsteadiness are warning signs. These symptoms indicate the nervous system is being overloaded and the treatment plan must be modified.
Worsening is not a sign of progress. Proper progression is.
Real Case Example (Anonymized)
Patient: 52-year-old school teacher
Complaint: Dizziness for 4 months, fear of turning in bed
History: Told it was “stress” and given general exercises
Neurological screening
Clinical findings:
Undiagnosed posterior canal BPPV
The most common form of BPPV, often missed without proper positional testing. It causes brief but intense vertigo during bed turns or head movements.
Neck stiffness contributing to instability
Restricted neck movement can disturb balance signals to the brain. This stiffness often worsens unsteadiness and delays recovery if not treated alongside vestibular care.
Treatment:
One repositioning maneuver
A specific therapeutic movement was performed to guide displaced inner ear crystals back to their correct position. This directly addressed the cause of positional vertigo.
Gentle balance retraining
Simple, controlled balance exercises were introduced to restore confidence and stability. Progression was gradual to avoid symptom flare-ups.
Neck mobility correction
Targeted neck movements and posture correction were used to improve mobility. This helped normalize balance input and reduce residual unsteadiness.
Outcome:
Spinning resolved in 2 sessions
The intense spinning sensation reduced rapidly after targeted treatment, with symptoms settling within just two therapy sessions. Early correction prevented recurrence and avoided prolonged discomfort.
Balance confidence returned over 3 weeks

When You Should Seek Medical Referral First (Red Flags)
Do NOT start vestibular therapy without medical review if you have:
- Sudden hearing loss
- Slurred speech or facial weakness
- Double vision
- New severe headache
- Fainting or blackouts
- Progressive neurological symptoms
These require urgent medical evaluation, not physiotherapy.
Read More:- Cost Of Physiotherapy In Ahmedabad

Common Home Mistakes That Delay Recovery
From real clinic experience:
Repeating random online vertigo exercises
Following unverified exercises without proper diagnosis can worsen symptoms or delay recovery. Vertigo management must be condition-specific and clinically guided.
Avoiding all movement out of fear
Complete rest increases balance sensitivity and slows vestibular adaptation. Safe, graded movement is essential for long-term recovery.
Overdoing exercises multiple times daily
Excessive repetition can overstimulate the vestibular system and trigger symptom flare-ups. Exercises should follow a prescribed frequency and intensity.
Ignoring neck posture and screen habits
Poor neck alignment and prolonged screen use can aggravate dizziness and balance issues. Postural correction is a key part of vertigo rehabilitation.
Stopping therapy too early once dizziness reduces
Early symptom relief does not mean full recovery. Incomplete therapy increases the risk of relapse and persistent balance problems.

What Recovery Realistically Looks Like
Honest answer:
- BPPV: Days to weeks
- Post-viral dizziness: 4–8 weeks
- Post-concussion: 6–12 weeks
- Migraine-related dizziness: Ongoing management, not cure
Progress is gradual but measurable when therapy is done correctly.

Choosing the Right Vestibular Physiotherapist
Look for someone who:
- Performs positional and eye movement testing
- Explains why you feel dizzy
- Adjusts exercises based on response
- Works with doctors when needed
- Does NOT rush or generalize care
Equipment matters less than clinical reasoning and experience.
Conclusion
Vestibular therapy can be life-changing —
but only when it is diagnosis-driven, patient-specific, and safely progressed.
If your dizziness has made you fearful, limited your independence, or confused by mixed advice — start with a proper evaluation, not random exercises.
Balance can be retrained.
Confidence can return.
But only with the right approach.
Vestibular rehabilitation therapy: FAQs
Q1. Is vestibular rehabilitation therapy suitable for all types of dizziness?
No. Vestibular therapy is effective only for specific balance-related diagnoses like BPPV or vestibular neuritis. Proper clinical assessment is essential before starting exercises.
Q2. Is it normal to feel slightly dizzy after vestibular exercises?
Mild, short-lasting dizziness can occur, especially early in treatment. Symptoms should settle within minutes to hours, not worsen over time.
Q3. How long does it usually take to recover with vestibular therapy?
Recovery time depends on the condition. BPPV may improve in days, while post-viral or post-concussion dizziness can take several weeks.
Q4. Can I do vestibular exercises from YouTube or the internet?
Random online exercises can delay recovery or worsen symptoms. Vestibular therapy must be tailored to your diagnosis and symptom response.
Q5. 5. When should I see a doctor before starting vestibular therapy?
If you have hearing loss, fainting, double vision, severe headache, or neurological symptoms, medical evaluation is required before physiotherapy.
References
About the Author

Dr. Hetal M Varia
After a rich experience of working in US healthcare as manager and licensed physiotherapist in US for last 11 years, she has returned home with a vision to become pioneer of Vestibular Therapy and specialized Parkinson physiotherapy in Ahmedabad. With her special skills and expertise in vertigo, Parkinson, balance and movement disorders therapy, Dr. Varia is committed to provide US standards of therapy services , compassionate and patient centered care to our people and community. With a vision of the world where everyone walks strong & steady, she intends to empower individuals with vestibular and neurological disorders through specialized care, rehabilitation & innovative therapies to improve mobility, balance & overall quality of life!