Physiotherapy vs Painkillers: What Actually Helps Recovery?
In my clinical work with patients in Ahmedabad, one pattern appears again and again. People are not choosing the “wrong” treatment. They are choosing temporary relief without understanding long-term recovery.
I commonly see situations like:
- A 38-year-old office worker taking NSAIDs daily for months for lower back pain.
- A parent who feels normal while on medication but worries when pain returns after missing a dose.
- A post-surgery patient resting too much because pain is controlled, while muscle strength slowly declines.
- An athlete avoids training because they believe pain always means structural damage.
The real problem is not painkillers or physiotherapy, but understanding why exercise-based rehabilitation often leads to better long-term recovery than temporary pain relief methods.
The problem is timing and understanding how the body heals.
This article explains when medication helps, when rehabilitation matters more, and how the two approaches can work together.
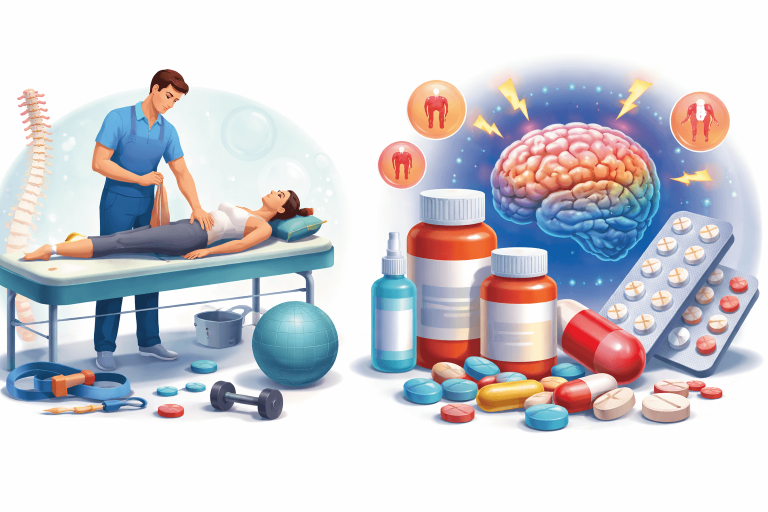
What Painkillers Actually Do
Pain medication changes how the body perceives pain, but it does not repair tissue. Common medications such as NSAIDs work by reducing inflammatory signals and altering how pain messages are processed in the nervous system. This can help patients move more comfortably in the early stages of injury.
However, pain relief alone does not:
rebuild weak muscles
Muscle strength returns only through progressive, structured exercise. Without resistance training and neuromuscular activation, weakened muscles remain deconditioned even if pain is reduced. Clinical rehabilitation focuses on gradual loading to restore real strength and function.
restore joint mobility
Joint stiffness improves through guided movement, stretching when appropriate, and controlled mobility exercises. Medication may reduce pain during movement, but it does not physically improve joint range of motion. Mechanical movement is necessary to regain flexibility and prevent long-term restriction.
improve movement patterns
After injury, people often develop protective habits like limping or guarding. Correcting these patterns requires assessment, motor retraining, and feedback. Painkillers do not retrain coordination or restore normal biomechanics.
increase tissue strength
Ligaments, tendons, and muscles adapt to gradual mechanical stress over time. Tissue healing and resilience improve through progressive loading — not through pain suppression alone. Over-reliance on medication without rehabilitation may even increase the risk of re-injury once activity resumes.

When Short-Term Medication Can Be Helpful
Medication can play an important role in the early phase of injury or surgery.
For example, doctors may recommend short-term medication when:
- inflammation is high during the first few days after injury
- pain prevents sleep or normal daily movement
- patients are recovering from surgery
- severe pain limits even gentle rehabilitation
In these situations, medication can actually support recovery by allowing early controlled movement, which is important for healing.
Medical organizations such as the World Health Organization emphasize the importance of maintaining safe movement during recovery from musculoskeletal conditions.
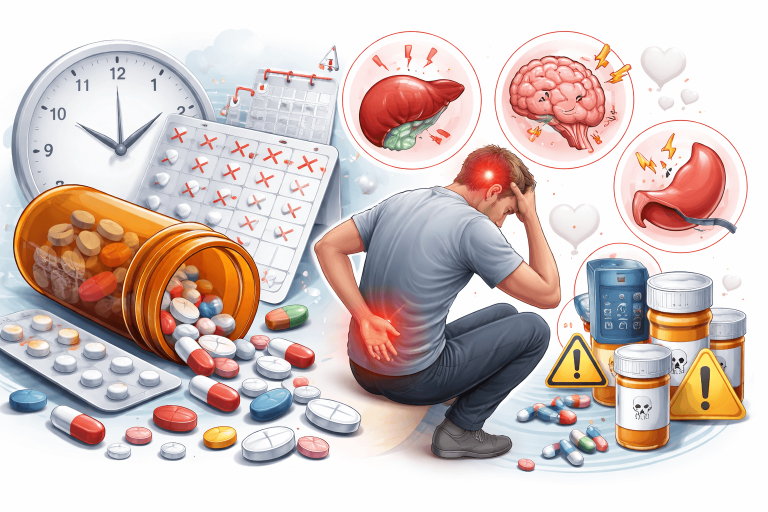
The Problem with Long-Term Reliance on Painkillers
In many chronic pain cases, I observe the following cycle:
- Pain increases
- Medication reduces symptoms
- Activity suddenly increases
- The tissue is not strong enough to handle the load
- Pain returns
- Medication restarts
Over time, the underlying physical capacity has not improved. The tissue remains sensitive, and the nervous system becomes more protective.
Long-term unsupervised NSAID use may also create additional risks such as stomach irritation or kidney strain, which is why doctors generally recommend the shortest effective duration of use.

What Physiotherapy Actually Changes
1. Tissue Adaptation
When muscles, tendons, and joints are exposed to gradually increasing load, the body responds by strengthening the involved structures. Collagen fibres reorganize, muscle strength improves, and joints become more stable. These changes take time typically several weeks but they create long-term resilience rather than temporary relief.
2. Nervous System Desensitization
Modern pain science shows that pain does not always equal structural damage. Sometimes the nervous system becomes overly protective after injury. Gradual exposure to safe movement helps the brain relearn that certain movements are not dangerous. Research summarized by the National Institutes of Health supports graded movement and exercise as key strategies in managing many chronic musculoskeletal pain conditions.
3. Movement Retraining
Pain often changes how people move.
For example, patients may:
stiffen surrounding muscles
When a joint hurts, nearby muscles tighten automatically to “guard” the area. While this protective response is normal, prolonged stiffness reduces blood flow, limits joint mobility, and increases fatigue. In clinical practice, we often see this in neck pain, low back pain, and shoulder injuries where muscle guarding becomes a major source of ongoing discomfort.
avoid certain ranges of motion
Patients commonly stop moving into positions that once caused pain like bending forward after a back strain or lifting the arm overhead after a shoulder injury. Avoidance may feel safe, but when medically unnecessary, it can lead to joint stiffness, reduced flexibility, and delayed recovery. A proper assessment helps determine which movements are truly unsafe and which simply need gradual reintroduction.
shift weight unevenly to reduce discomfort
With knee, hip, ankle, or back pain, people often put more weight on the “good” side without realizing it. Over time, this imbalance can overload other joints and create secondary pain. For example, untreated limping after a knee injury frequently leads to hip or lower back strain.
Physiotherapy helps restore:
balanced movement patterns
After pain or injury, the body often develops compensations, overusing some muscles while underusing others. Physiotherapy identifies these imbalances through movement assessment and corrects them with targeted exercises. Restoring balanced movement reduces strain on joints, improves efficiency, and lowers the risk of re-injury. This approach is based on biomechanics and real clinical observation, not generic exercise advice, which is why it is important to find the right physiotherapy care for your condition to ensure proper assessment and individualized treatment.
joint stability
Joint stability is not just about “tight” muscles — it depends on coordinated muscle activation, ligament support, and proper joint alignment. Through progressive strengthening and neuromuscular training, physiotherapy improves the body’s ability to control joints during movement. This is especially important in conditions like ligament injuries, recurrent sprains, shoulder instability, and post-surgical recovery.
confidence during daily activities
Many patients hesitate to bend, lift, walk long distances, or climb stairs after experiencing pain. This fear of movement can slow recovery. Guided rehabilitation gradually exposes the body to safe, controlled activity, rebuilding both physical capacity and psychological confidence. When patients understand what is safe and why they move more naturally and recover more completely.

A Practical Decision Framework
In real clinical practice, treatment decisions follow a step-by-step process.
Step 1: Rule Out Red Flags
Before starting rehabilitation, it is important to identify serious medical causes such as fractures, infections, or significant neurological problems. Symptoms like progressive weakness, loss of bladder control, fever with severe pain, or unexplained weight loss require immediate medical evaluation.
Step 2: Acute Phase (First Week)
During the early stage of injury:
short-term medication may be used if prescribed
If advised by a doctor, a brief course of pain-relieving or anti-inflammatory medication may help manage excessive pain and swelling. This is typically limited to a short duration and used alongside physical management — not as a replacement for proper rehabilitation. Clinical judgment is important to avoid masking symptoms that guide safe progression.
gentle movement is encouraged
Once serious damage is ruled out, controlled and pain-free movement is usually beneficial. Gentle mobility improves circulation, reduces joint stiffness, and supports tissue healing. Evidence and real-world rehabilitation experience show that complete rest often delays recovery in uncomplicated musculoskeletal injuries.
aggressive exercise is avoided
High-load strengthening, deep stretching, or intense activity too early can aggravate inflammation and delay healing. In the acute phase, tissues are biologically vulnerable. Rehabilitation must respect healing timelines and gradually progress based on symptoms, swelling, and functional improvement.
Step 3: Recovery Phase (1–6 Weeks)
As inflammation decreases, the focus gradually shifts from symptom relief to improving movement and strength. Medication may be reduced while rehabilitation exercises increase.
Step 4: Strength and Adaptation
At this stage, progressive strengthening becomes the main strategy. Pain reduction becomes a secondary outcome, while functional improvement becomes the primary goal.
Step 5: Long-Term Prevention
Maintaining strength and mobility two or three times per week helps ensure that the body’s physical capacity remains higher than the demands of daily life. This reduces the risk of recurring pain episodes.

Real Clinical Examples
Chronic Desk Worker
A 42-year-old professional came to our clinic after using NSAIDs for six months to manage persistent lower back pain.
The plan included:
- gradual reduction of medication
- low-load core endurance training
- weekly monitoring of symptoms and activity levels
After twelve weeks:
- daily medication was no longer required
- sitting tolerance improved from 30 minutes to nearly three hours
- only mild occasional stiffness remained
The improvement came from consistent progression rather than instant relief.

Recreational Athlete with Ankle Injury
Another patient presented with acute ankle swelling after a sports injury.
Management included:
short-term medication for five days
Under medical supervision, a brief course of anti-inflammatory medication was used to help control pain and excessive inflammation during the acute phase. This was limited to a few days to avoid masking symptoms or delaying tissue healing. Medication was used as support — not as the primary treatment.
early mobility exercises
Once serious injury was ruled out, gentle, pain-free ankle movements were started early. Controlled mobility improves circulation, reduces stiffness, and prevents joint restriction. Research and clinical experience both show that prolonged immobilization can delay recovery in most uncomplicated sprains.
progressive strength training
As swelling reduced, rehabilitation shifted toward strengthening the ankle stabilizers especially the peroneal muscles, calf complex, and intrinsic foot muscles. Balance and proprioception exercises were gradually introduced to restore joint stability and reduce the risk of recurrent sprains, which are common when rehab is incomplete.
Conclusion
The question is not physiotherapy vs painkillers.
The real question is what stage of recovery are you in — and what does your body need right now?
Painkillers can be helpful in the short term. They reduce discomfort, calm excessive inflammation, and may allow you to begin moving earlier. When prescribed appropriately, they support recovery. But medication does not rebuild strength. It does not restore joint mobility. It does not retrain movement patterns. And it does not increase long-term tissue capacity.
Physiotherapy focuses on what creates lasting change progressive loading, movement correction, nervous system desensitization, and functional rebuilding. These adaptations take time, but they address the root cause rather than just the symptoms.
In real clinical practice, the most effective approach is often combination and timing:
- Short-term symptom control when necessary
- Early guided movement
- Gradual strengthening
- Long-term capacity building
Recovery is not about eliminating pain instantly. It is about restoring the body’s ability to tolerate life’s physical demands safely and confidently. When patients understand this difference, they stop chasing temporary relief and start building durable recovery.
Physiotherapy vs Painkillers - FAQs
Q1.Can I take painkillers during physiotherapy?
Q2. Will pain increase when I stop medication?
Q3. Is pain during exercise harmful?
Q4. Should I rest until the pain is completely gone?
Q5. How do I know I’m improving?
References
About the Author

Dr. Hetal M Varia
After a rich experience of working in US healthcare as manager and licensed physiotherapist in US for last 11 years, she has returned home with a vision to become pioneer of Vestibular Therapy and specialized Parkinson physiotherapy in Ahmedabad. With her special skills and expertise in vertigo, Parkinson, balance and movement disorders therapy, Dr. Varia is committed to provide US standards of therapy services , compassionate and patient centered care to our people and community. With a vision of the world where everyone walks strong & steady, she intends to empower individuals with vestibular and neurological disorders through specialized care, rehabilitation & innovative therapies to improve mobility, balance & overall quality of life!