Physiotherapy Treatment For Ligament Injury
Physiotherapy Treatment For Ligament Injury: A Clinically Guided, Patient-Focused Recovery Approach. Ligament injuries are common, but they are often misunderstood and poorly managed.
In my clinical practice, I regularly see patients who were told to “just rest,” were overtreated with machines, or returned to activity too early—only to develop chronic instability, repeated injuries, or long-term pain.
Physiotherapy, when done with proper assessment and clinical reasoning, plays a critical role in ligament healing, joint stability, and safe return to function. But it must be timed correctly, structured properly, and tailored to the individual injury.
This article will help you understand:
- What a ligament injury really means
- When physiotherapy helps—and when it doesn’t
- What proper treatment looks like step by step
- How long recovery realistically takes
- Mistakes that delay healing
- Red flags you should never ignore
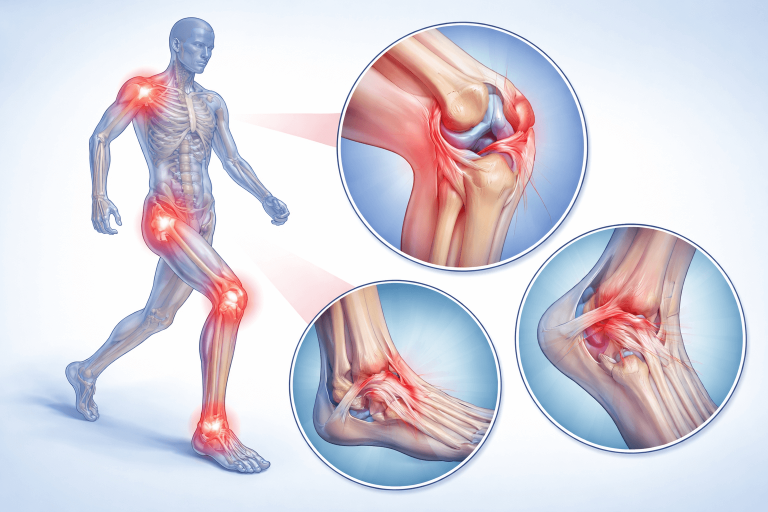
What Is a Ligament Injury?
Ligaments are strong connective tissues that connect one bone to another and stabilize joints. When a ligament is overstretched or torn due to trauma or sudden force, it results in a sprain.
Common ligament injuries include:
Ankle ligament sprains
Ankle ligament sprains usually happen after a twist or misstep and can make walking feel unstable. Proper assessment and early physiotherapy help control swelling, restore balance, and prevent repeated sprains that many people experience later.
Knee ligaments (ACL, MCL, PCL)
Knee ligament injuries often cause pain, swelling, or a feeling that the knee may “give way.” Treatment depends on the ligament involved, injury severity, and your activity level, with physiotherapy playing a key role both with and without surgery.
Wrist and thumb ligaments
These injuries commonly occur after falls or sudden force on the hand and can affect grip strength and daily tasks. Early diagnosis and guided rehabilitation are important to avoid long-term stiffness or weakness.
Shoulder ligaments
Shoulder ligament injuries may lead to pain, instability, or difficulty lifting the arm. Physiotherapy focuses on restoring controlled movement and shoulder stability rather than forcing painful exercises too early.
Cervical or lumbar ligament strain after accidents
Neck or lower back ligament strain often follows sudden impact, such as a road traffic accident. Gentle, well-timed physiotherapy helps reduce stiffness, restore movement confidence, and prevent chronic pain from developing.
Grades of Ligament Injury
Understanding severity is essential because treatment decisions depend on it:
- Grade 1 (Mild): Microscopic tears, pain but no instability
- Grade 2 (Moderate): Partial tear, swelling, weakness, joint looseness
- Grade 3 (Severe): Complete rupture, clear instability, often needs surgical opinion

Common Symptoms Patients Experience
Patients usually report a mix of:
- Pain around the joint
- Swelling and stiffness
- Difficulty bearing weight or using the limb
- Feeling of “giving way” or instability
- Reduced confidence in movement
A key clinical point:
Pain reduction does NOT mean the ligament has healed. Ligament healing takes longer than muscle recovery.
Why Physiotherapy Is Essential for Ligament Injuries
Ligaments have limited blood supply, so they heal slowly and require controlled loading not complete rest and not aggressive exercise.
Physiotherapy helps by:
- Protecting healing tissue in early stages
- Restoring joint movement safely
- Re-educating muscles that protect the joint
- Preventing long-term instability and repeat injury
- Guiding a safe return to work, sport, or daily activity
In clinical practice, patients who skip proper rehabilitation often return later with:
- Chronic pain
- Recurrent sprains
- Early joint degeneration

Step-by-Step Physiotherapy Approach
Phase 1: Acute Protection Phase (First 1–2 Weeks)
Goal: Control pain, swelling, and prevent further damage
Physiotherapy focuses on:
- Joint protection and activity modification
- Swelling control (not overuse of heat)
- Gentle pain-free movements
- Isometric muscle activation
- Guidance on walking, bracing, or taping if needed
What does NOT help here:
- Aggressive stretching
- Deep massage on the ligament
- Forcing movements through pain
Phase 2: Controlled Mobility & Strength (2–6 Weeks)
Goal: Restore movement and joint support
- Gradual range-of-motion exercises
- Strengthening muscles around the joint
- Balance and proprioception training
- Correcting faulty movement patterns
Clinical insight:
Many ligament injuries fail to heal properly because balance and neuromuscular control are ignored.
Phase 3: Functional & Return-to-Activity Training
Goal: Prepare the joint for real-life demands
Treatment becomes more specific:
- Activity-based strengthening
- Direction-change control
- Load tolerance training
- Sport- or work-specific drills (when appropriate)
Only when strength, control, and confidence return, should full activity resume.
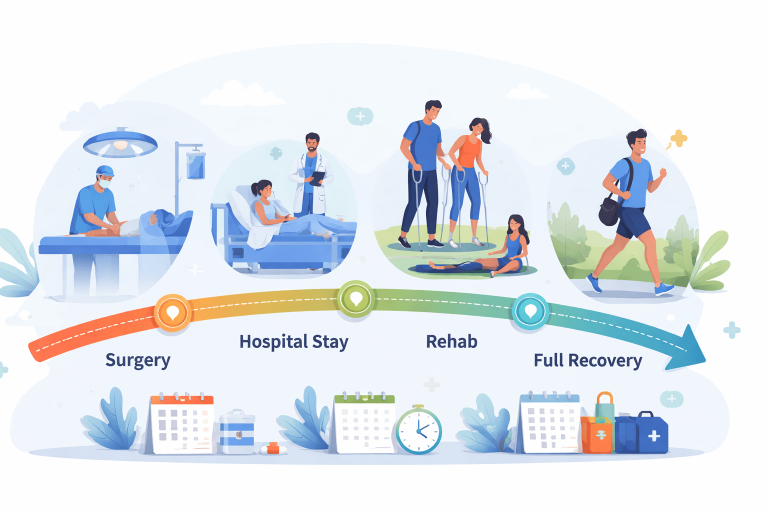
Realistic Recovery Timeline
Recovery depends on:
Injury grade
The severity of the ligament injury directly affects how long healing takes. Mild injuries recover faster, while partial or complete tears need more time and carefully guided rehabilitation to restore joint stability—making it essential to restore movement with physiotherapy in Ahmedabad for safe and effective recovery.
Joint involved
Different joints heal at different speeds because of their structure and load demands. Weight-bearing joints like the knee or ankle usually take longer than smaller joints such as the wrist or fingers.
Age and health status
Healing capacity changes with age and overall health. Conditions like diabetes, poor fitness, or smoking can slow tissue repair and require a more cautious rehabilitation plan.
Quality of rehabilitation
Recovery depends not just on exercises, but on doing the right exercises at the right time. Clinically guided physiotherapy reduces re-injury risk and helps restore confidence, strength, and control safely.
Typical timelines:
- Grade 1: 2–4 weeks
- Grade 2: 6–10 weeks
- Grade 3: 3–6 months (sometimes longer, especially post-surgery)
Rushing recovery increases re-injury risk significantly.

Real-World Case Example
A middle-aged office worker came with a recurrent ankle sprain history. He had taken rest and painkillers multiple times but never underwent structured physiotherapy, including guided exercises for ligament recovery, which are essential to restore stability and prevent repeated injuries.
Clinical findings showed:
- Poor ankle balance
- Weak peroneal muscles
- Delayed reaction time
After 6 weeks of focused rehabilitation emphasizing balance retraining and joint control, his episodes of instability stopped, and he returned to walking confidently without fear. This is a common story in clinical practice.
When Physiotherapy May Not Be Enough
Physiotherapy alone may not be sufficient if:
- There is a complete ligament rupture with instability
- Locking or catching is present in the joint
- Symptoms worsen despite proper rehab
- There is associated fracture or cartilage injury
In such cases, orthopedic evaluation and imaging are necessary.

Red Flags That Need Immediate Medical Attention
Seek urgent evaluation if you experience:
- Severe swelling within hours of injury
- Inability to bear weight
- Joint deformity
- Numbness or tingling
- Repeated joint “giving way”
These signs may indicate serious structural damage.
Common Home Mistakes That Delay Healing
From clinical experience, the most damaging mistakes include:
- Resuming activity as soon as pain reduces
- Overstretching a healing ligament
- Ignoring balance and control exercises
- Using heat too early
- Self-medicating without assessment
Who Is Physiotherapy Right For?
Physiotherapy is ideal for:
Mild to moderate ligament injuries
These injuries often heal well with timely, guided physiotherapy. Structured care helps reduce pain, restore joint control, and prevent the injury from becoming a long-term problem.
Post-surgical ligament reconstruction
After surgery, physiotherapy is essential to regain movement, strength, and joint stability. Rehabilitation is progressed carefully to protect the repair while helping patients return to daily activities safely.
Recurrent sprains
Repeated sprains usually mean the joint has not fully recovered or lacks proper control. Physiotherapy focuses on strengthening, balance training, and movement correction to break the cycle of re-injury.
Patients aiming to return to active life safely
For people who want to resume work, exercise, or sports, physiotherapy helps rebuild confidence and functional strength. The goal is a safe return without pushing the joint before it is ready.
It may not be suitable as the only treatment for:
Unstable complete ruptures without medical review
When a ligament is completely torn and the joint feels unstable, physiotherapy alone is not enough at the start. These cases require proper medical evaluation and imaging, as delayed or inappropriate treatment can lead to long-term instability and joint damage.
Final Clinical Advice
Ligament injuries are not just about pain relief—they are about joint stability, confidence, and long-term health.
Proper physiotherapy:
- Respects healing timelines
- Uses clinical reasoning, not protocols
- Focuses on movement quality, not machines
If managed correctly, most ligament injuries recover well. If managed poorly, they often return.
Physiotherapy Treatment For Ligament Injury - FAQs
Q1. How many sessions are usually required?
Q2. Is physiotherapy effective for Parkinson’s?
Q3. What is the average physiotherapy cost in Ahmedabad?
Q4. Can vertigo be cured permanently?
Q5. How do I verify a physiotherapist’s credentials?
References
About the Author

Dr. Hetal M Varia
After a rich experience of working in US healthcare as manager and licensed physiotherapist in US for last 11 years, she has returned home with a vision to become pioneer of Vestibular Therapy and specialized Parkinson physiotherapy in Ahmedabad. With her special skills and expertise in vertigo, Parkinson, balance and movement disorders therapy, Dr. Varia is committed to provide US standards of therapy services , compassionate and patient centered care to our people and community. With a vision of the world where everyone walks strong & steady, she intends to empower individuals with vestibular and neurological disorders through specialized care, rehabilitation & innovative therapies to improve mobility, balance & overall quality of life!