How Physiotherapy Helps Chronic Pain Relief
As a physiotherapist treating chronic pain patients every day, one thing becomes very clear very quickly: chronic pain is not just “long-lasting pain.” It is a condition that affects movement, confidence, sleep, emotions, and trust in one’s own body.
Many patients who come to my clinic have already tried painkillers, rest, scans, injections, or multiple opinions. What they often lack is a clear explanation of why the pain persists and what can realistically help.
This article explains how physiotherapy helps chronic pain, who benefits most, where its limits lie, and how patients can make informed decisions without false promises.
Understanding Chronic Pain: What Patients Often Don’t Get Told
Clinically, pain is considered chronic when it lasts longer than 3 months — even after tissue healing should have occurred. But chronic pain is not always a sign of ongoing damage.
From clinical assessment, chronic pain usually involves a combination of:
- Altered muscle activation and weakness
- Reduced joint mobility or movement avoidance
- Nervous system sensitization (pain signals become overactive)
- Fear of movement and loss of confidence
- Poor sleep, stress, and fatigue
Important clinical truth:
A scan may show changes, but pain severity does not always match imaging findings. Treatment decisions must be based on function and movement, not reports alone.
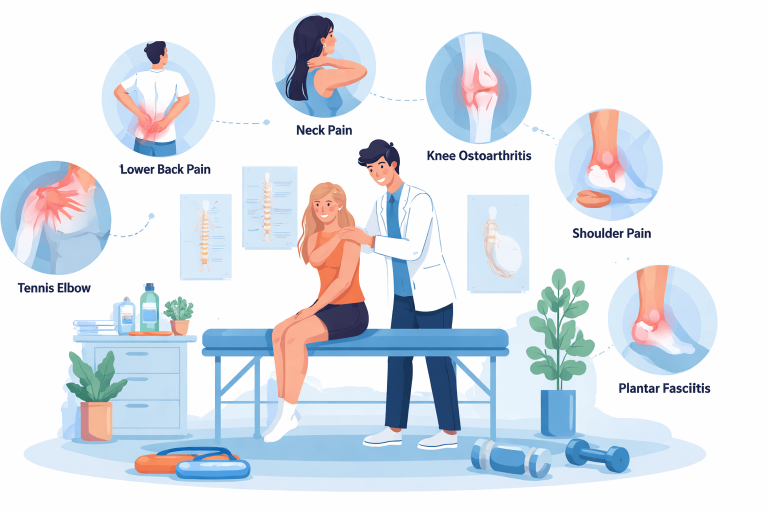
Common Chronic Pain Conditions Seen in Physiotherapy Clinics
Physiotherapy commonly helps patients with:
Chronic low back or neck pain
Pain lasting months is often linked to reduced movement, muscle imbalance, and fear of activity rather than ongoing damage. Physiotherapy focuses on restoring safe movement, strength, and confidence to prevent repeated flare-ups—this is why physiotherapy for chronic pain relief in Ahmedabad plays a key role in addressing the root cause and supporting long-term recovery.
Osteoarthritis-related pain
Arthritis pain is not just “wear and tear” but also stiffness, weakness, and altered joint loading. Physiotherapy helps by improving joint mobility, muscle support, and daily function without overloading painful joints.
Fibromyalgia (as part of a multidisciplinary approach)
Fibromyalgia involves widespread pain and nervous system sensitivity rather than tissue injury. Gentle, graded physiotherapy combined with education helps reduce flare-ups and improve energy, movement tolerance, and quality of life.
Post-surgical persistent pain
Pain that continues after surgery often results from stiffness, weakness, or altered movement patterns. Physiotherapy supports safe recovery by restoring strength, mobility, and functional use while respecting surgical healing timelines.
Shoulder, knee, or hip pain lasting months
Long-standing joint pain is commonly related to poor load management and muscle weakness. Physiotherapy targets controlled strengthening and movement retraining to reduce pain and improve daily activity tolerance.
Work-related or postural pain syndromes
Prolonged sitting, repetitive tasks, or poor posture can overload muscles and joints over time. Physiotherapy addresses posture, workstation habits, and movement strategies to prevent recurring pain and work-related strain.
Common Chronic Pain Conditions Seen in Physiotherapy Clinics
1. Accurate Clinical Assessment — Not Guesswork
The first and most important step is understanding:
- What movements worsen or ease pain
- How the body compensates
- Muscle strength, endurance, and coordination
- Nervous system sensitivity
- Daily activity limitations
This assessment guides safe and targeted treatment, not random exercises.
2. Reducing Pain Without Over-Reliance on Medication
Physiotherapy reduces pain by:
- Improving joint movement and load distribution
- Normalizing muscle activation
- Calming an over-sensitive nervous system through graded movement
- Correcting protective but harmful movement patterns
What does not help long-term:
- Prolonged rest
- Repeated painkillers without rehabilitation
- Passive treatments alone
Pain relief is a by-product of better movement, not the only goal.
3. Graded Movement Therapy: Rebuilding Trust in the Body
Many chronic pain patients fear movement — understandably.
Physiotherapy uses graded exposure, meaning:
Movements start well within tolerance
Physiotherapy begins with movements that feel safe and manageable, not painful or forced. This helps protect sensitive tissues and builds trust in the body’s ability to move again.
Progression is slow and planned
Exercises are increased gradually based on how the body responds, not on rigid timelines. This reduces setbacks and allows steady improvement without overwhelming healing tissues.
Pain flares are anticipated and managed, not feared
Temporary symptom increases can occur during recovery and do not mean harm. Physiotherapy teaches patients how to respond to flares calmly, adjust activity, and continue progressing safely.
4. Strength, Endurance, and Functional Retraining
Chronic pain weakens muscles over time.
Treatment focuses on:
- Strengthening without flare-ups
- Improving endurance for daily tasks
- Training real-life movements (sitting, walking, lifting)
The goal is independence, not endless therapy sessions.
5. Nervous System Education and Pain Understanding
One of the most powerful tools in chronic pain care is education.
Patients learn:
- Why pain can persist without damage
- Why “hurt does not always mean harm”
- How stress, sleep, and fear influence pain
This knowledge alone often reduces pain intensity and anxiety.

A Real Clinical Example (Anonymized)
A 45-year-old woman with chronic neck and shoulder pain for 2 years had normal scans but severe pain and stiffness. She avoided movement due to fear of worsening damage.
Treatment focused on:
Gentle mobility
Early movement helps reduce stiffness and improve circulation without stressing painful tissues. Physiotherapy introduces safe, controlled motions that keep joints flexible while respecting pain limits.
Gradual strengthening
Strength is rebuilt step by step to support joints and improve daily function. Exercises are carefully progressed to avoid flare-ups and build confidence in movement, not fear.
Posture and work habit changes
Small daily habits often contribute more to pain than one-time injuries. Physiotherapy helps patients adjust sitting, standing, lifting, and work routines to reduce ongoing strain on the body, making chronic pain management through physiotherapy an effective approach for long-term relief and improved function.
Pain education
Understanding why pain occurs reduces fear and unnecessary activity avoidance. Physiotherapists explain what pain means, what is safe to do, and how to respond to symptoms confidently.

What Physiotherapy Can and Cannot Do in Chronic Pain
Physiotherapy CAN:
- Improve function and quality of life
- Reduce pain intensity over time
- Restore confidence in movement
- Reduce dependence on medication
Physiotherapy CANNOT:
- Offer instant or guaranteed cures
- Eliminate pain in every case
- Replace medical care when red flags exist
Honest expectations protect patient trust.

When Physiotherapy May NOT Be Enough Alone
Immediate medical evaluation is needed if there is:
- Progressive weakness or numbness
- Loss of bladder or bowel control
- Unexplained weight loss or night pain
- Fever, infection, or trauma history

Common Home Mistakes That Worsen Chronic Pain
From daily clinical practice, common errors include:
- Avoiding movement completely
- Doing random online exercises
- Pushing through severe pain
- Stopping therapy once pain reduces
- Ignoring sleep, stress, and posture

Step-by-Step: What Patients Should Do
Step 1: Get a proper physiotherapy assessment
Step 2: Start gentle pain-modulating movement
Step 3: Progress to strength and functional training
Step 4: Learn self-management strategies
Step 5: Maintain activity to prevent relapse

How Long Does Chronic Pain Recovery Take?
Recovery depends on:
- Duration of pain
- Underlying condition
- Consistency with therapy
- Lifestyle factors
Typical timelines:
- Early chronic pain: 6–8 weeks
- Long-standing pain: 8–16 weeks or longer
- Maintenance: ongoing self-management
Final Physiotherapist’s Perspective
Chronic pain does not mean your body is broken. It means your system needs careful retraining, not force or fear.
Good physiotherapy:
- Respects your limits
- Explains the “why” behind treatment
- Adapts as you improve
- Focuses on long-term independence
If your care plan feels rushed, unclear, or fear-based — ask questions.
Your recovery should be guided, not guessed.
How Physiotherapy Helps Chronic Pain Relief - FAQs
Q1.Can physiotherapy really help with long-term chronic pain?
Q2.Will physiotherapy increase my pain at the beginning?
Q3.How long does it take to see improvement in chronic pain?
Q4.Is physiotherapy safe for chronic pain conditions?
Q5.Do I need scans or tests before starting physiotherapy?
References
About the Author

Dr. Hetal M Varia
After a rich experience of working in US healthcare as manager and licensed physiotherapist in US for last 11 years, she has returned home with a vision to become pioneer of Vestibular Therapy and specialized Parkinson physiotherapy in Ahmedabad. With her special skills and expertise in vertigo, Parkinson, balance and movement disorders therapy, Dr. Varia is committed to provide US standards of therapy services , compassionate and patient centered care to our people and community. With a vision of the world where everyone walks strong & steady, she intends to empower individuals with vestibular and neurological disorders through specialized care, rehabilitation & innovative therapies to improve mobility, balance & overall quality of life!