Can Physiotherapy Cure Slip Disc Without Surgery?
When someone is told they have a “slip disc,” the first reaction is usually fear.
- “Will I need surgery?”
- “Is my spine damaged permanently?”
- “Will this come back again?”
In my clinical practice, I’ve seen hundreds of patients walk in believing surgery is inevitable—simply because their MRI showed a disc bulge or herniation.
Here’s the honest answer: In most cases, yes — physiotherapy can successfully treat slip disc without surgery. But only when it is done correctly, systematically, and based on proper assessment.
Let’s break this down clearly.
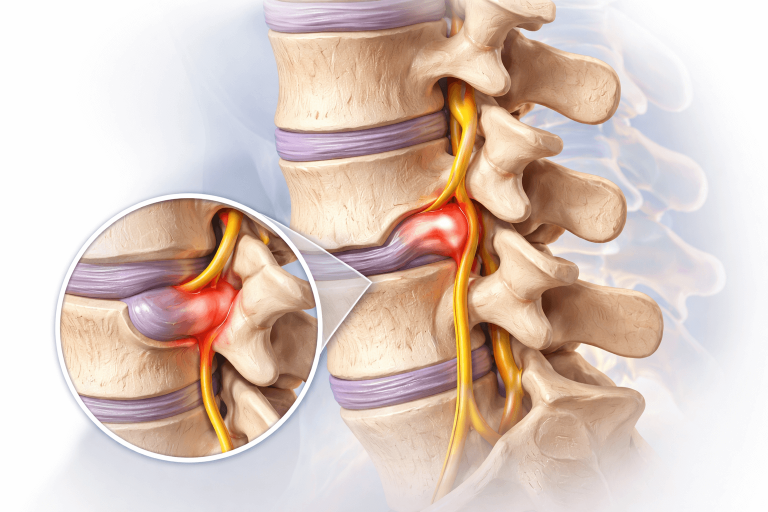
First, What Is a Slip Disc — Really?
The term “slip disc” is misleading. Discs do not actually slip out.
What usually happens is:
The disc bulges
A disc bulge means the outer layer of the spinal disc extends slightly beyond its normal boundary. Many people have bulges without symptoms, and when pain is present, it often responds well to structured physiotherapy rather than immediate surgery.
Or part of it protrudes outward
A disc protrusion occurs when inner disc material pushes outward but remains contained. With proper assessment and guided rehabilitation, symptoms can often be managed effectively without invasive treatment.
Sometimes it irritates a nearby nerve
When a disc irritates a nerve, it may cause radiating pain, tingling, or numbness. In many cases, reducing inflammation and improving spinal control through physiotherapy for slip disc without surgery helps calm the nerve and restore function safely.
Pain often comes more from inflammation and nerve sensitivity than from structural damage itself. This is important – because inflammation and sensitivity can be reduced without surgery.

When Is Surgery Actually Needed?
Before we talk about physiotherapy, we must be honest.
Surgery is necessary when:
- There is progressive muscle weakness
- Loss of bowel or bladder control
- Severe nerve compression not responding to care
- Major spinal instability
These cases are a minority. Most patients fall into the manageable category, not the emergency category.
Why Many Slip Discs Heal Without Surgery
The body has a natural healing ability, especially when supported with effective pain relief treatments in Ahmedabad that reduce stress on the affected tissues and promote recovery.
Research shows that:
Many disc herniations shrink over time
Research shows that the body can gradually reabsorb part of a disc herniation. With proper guidance and activity modification, symptoms often improve as natural healing progresses.
Inflammation settles gradually
Pain from a slip disc is often driven by inflammation rather than permanent damage. As irritation reduces through controlled movement and load management, discomfort typically decreases step by step.
Nerves calm down with guided movement
Sensitive nerves respond well to graded, safe movement instead of prolonged rest. Structured physiotherapy helps reduce nerve irritation while restoring normal function without aggressive intervention.
The problem is not the disc alone. It is often:
- Muscle weakness
- Poor lifting mechanics
- Prolonged sitting habits
- Core deconditioning
- Fear of movement
Surgery doesn’t fix these root causes. Physiotherapy does.
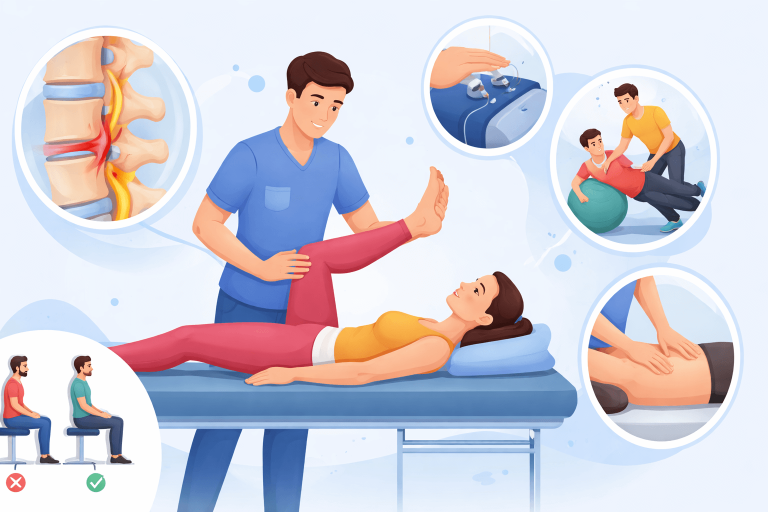
How Physiotherapy Treats Slip Disc — Step by Step
Step 1: Precise Mechanical Assessment
Not every slip disc behaves the same.
We assess:
- Direction of pain
- Movements that worsen or reduce symptoms
- Nerve involvement
- Strength and reflex changes
This determines the treatment plan. Generic exercises from YouTube often worsen symptoms because they ignore this step.
Step 2: Pain Reduction Without Bed Rest
Old advice recommended weeks of rest. That approach causes stiffness and weakness.
Instead, we:
- Use directional exercises
- Apply nerve mobility techniques
- Reduce inflammation safely
- Maintain controlled movement
Movement is medicine — when prescribed correctly.
Step 3: Nerve Desensitization
Sciatic pain often feels severe, but nerves can calm down.
Through:
Graded loading
Graded loading means gradually reintroducing movement and strength exercises in a controlled manner. This helps tissues adapt safely, reduces pain sensitivity, and rebuilds confidence without overstraining the spine.
Neural mobilization
Neural mobilization involves gentle, specific movements designed to improve nerve flexibility and reduce irritation. When performed correctly, it can ease radiating pain without aggressive stretching or force.
Posture correction
Posture correction focuses on improving how you sit, stand, and move during daily activities. Small adjustments in alignment and muscle control often reduce repeated stress on the spine and support long-term recovery.
Step 4: Core Stability & Load Correction
This is where long-term results are built.
We restore:
- Deep abdominal activation
- Hip strength
- Spine endurance
- Lifting mechanics
Without this phase, recurrence risk remains high.
Step 5: Fear Removal & Confidence Building
Many patients stop bending, sitting, or lifting due to fear. But fear increases muscle guarding. Education is part of treatment. When patients understand their spine is strong, recovery accelerates.
Real Case Examples From Practice
Case 1: 38-Year-Old IT Professional
- Severe leg pain
- MRI showed L4-L5 disc protrusion
- Advised surgery elsewhere
Treatment:
- Directional exercises
- Postural correction
- Progressive core training
Result:
Pain reduced in 4 weeks
Returned to office work
No surgery required
Case 2: 52-Year-Old Homemaker
- Radiating pain for 3 months
- Could not stand for long
Treatment:
- Nerve glides
- Hip strengthening
- Functional retraining
Result:
Pain centralized
Mobility restored
Independent daily activity resumed
Common Mistakes That Delay Recovery
From clinical experience, these worsen outcomes:
- Complete bed rest
- Heavy belt dependency
- Random online exercises
- Ignoring hip strength
- Returning to gym too early
- Focusing only on pain, not function
Slip disc recovery requires strategy — not shortcuts.
Can Physiotherapy “Cure” Slip Disc?
Important clarification:
Physiotherapy may not “remove” the disc bulge on MRI immediately.
But it can:
- Eliminate pain
- Restore normal life
- Prevent recurrence
- Avoid surgery
For most patients, that is what truly matters.
How Long Does Recovery Take?
- Mild cases: 2–4 weeks
- Moderate cases: 4–8 weeks
- Chronic cases: 8–12 weeks structured rehab
Consistency matters more than speed.
How to Know If You Are Improving
Positive signs include:
- Leg pain reducing first
- Pain centralizing toward back
- Improved sitting tolerance
- Reduced morning stiffness
- Better walking endurance
Progress should be steady, not dramatic.
When Surgery Should Still Be Considered
If despite structured physiotherapy:
Weakness worsens
If muscle strength in the leg or foot continues to decline despite treatment, it may indicate increasing nerve compression and requires urgent medical reassessment.
Pain becomes intolerable
Severe, unmanageable pain that does not improve with structured care may signal the need for further investigation or specialist consultation.
Neurological signs progress
Worsening numbness, loss of coordination, or changes in bowel or bladder control are serious warning signs that demand immediate medical evaluation.
Why I Recommend Trying Physiotherapy First
From years of treating spinal cases:
- Many patients improve without surgery
- Those who need surgery recover better after pre-rehab
- Strong muscles protect the spine long-term
- Confidence reduces recurrence
Surgery changes structure. Rehabilitation changes behavior and resilience. Both have value — timing matters.
Final Thoughts
A slip disc diagnosis is not a life sentence. Most cases respond well to:
- Guided movement
- Strength rebuilding
- Education
- Progressive loading
The key is proper evaluation, not panic. If you are facing a surgery recommendation, ask:
Have I completed a structured physiotherapy program first?
In many cases, the answer can change your outcome completely.
Can Physiotherapy Cure Slip Disc Without Surgery? - FAQs
Q1.Can physiotherapy really treat a slip disc without surgery?
Q2.How long does it take for a slip disc to heal with physiotherapy?
Q3. Is complete bed rest necessary for a slip disc?
Q4.When is surgery required for a slip disc?
Q5. Can slip disc pain come back after physiotherapy?
References
About the Author

Dr. Hetal M Varia
After a rich experience of working in US healthcare as manager and licensed physiotherapist in US for last 11 years, she has returned home with a vision to become pioneer of Vestibular Therapy and specialized Parkinson physiotherapy in Ahmedabad. With her special skills and expertise in vertigo, Parkinson, balance and movement disorders therapy, Dr. Varia is committed to provide US standards of therapy services , compassionate and patient centered care to our people and community. With a vision of the world where everyone walks strong & steady, she intends to empower individuals with vestibular and neurological disorders through specialized care, rehabilitation & innovative therapies to improve mobility, balance & overall quality of life!