Nerve Problem vs Muscle Problem: Key Differences You Should Know
Pain can be confusing—especially when it lingers, changes character, or doesn’t respond to rest. Many patients visiting Varia Physiotherapy Clinic in Ahmedabad often ask a very important question: “Is my pain coming from a nerve or a muscle?”
Understanding the difference between a nerve problem vs muscle problem: key differences you should know can make a significant impact on your recovery. It determines not just what treatment you need, but how quickly and effectively you heal.
If you’re between 30–65 years old and dealing with persistent back pain, neck stiffness, tingling in your limbs, or unexplained weakness, this guide is written with your experience in mind.
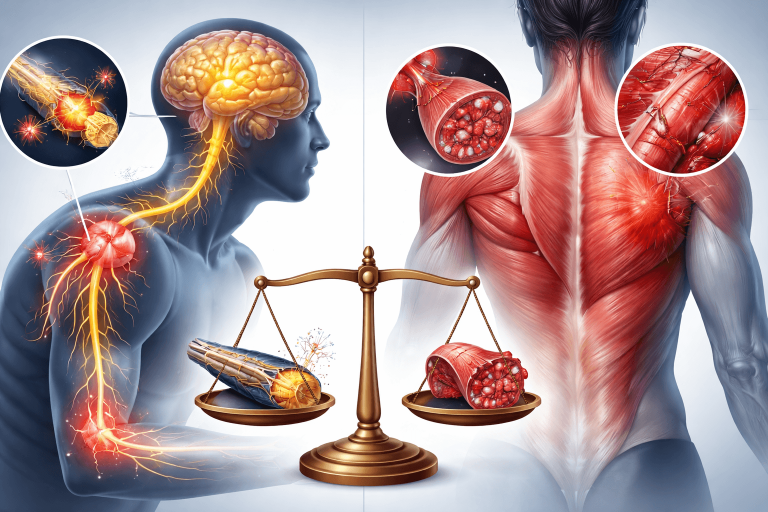
Why It’s Important to Differentiate Between Nerve and Muscle Problems
Pain is your body’s signal—but not all pain is the same. At our clinic in Ahmedabad, we frequently see patients who have been treating the wrong cause for months. A muscle issue treated like a nerve problem (or vice versa) can delay recovery and increase discomfort, which is why it’s important to get expert guidance for rehabilitation to identify the exact cause and start the right treatment.
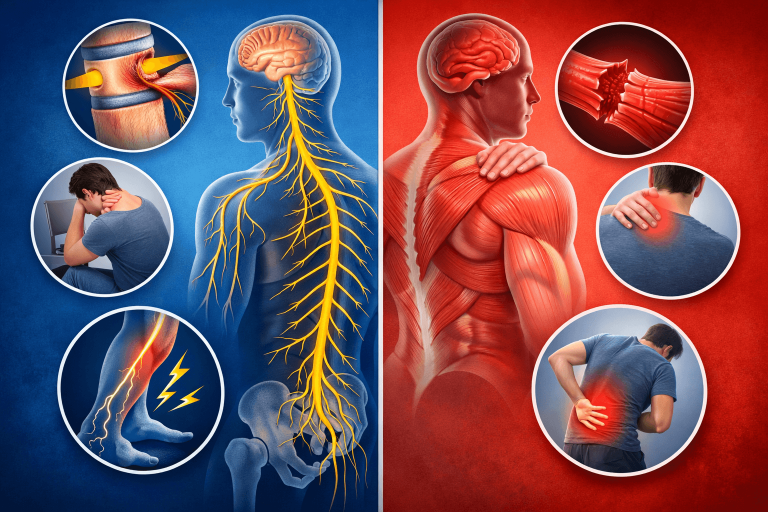
Muscle Problems (Musculoskeletal Pain)
These arise from:
Overuse or Strain
This happens when a muscle is used repeatedly without enough rest, often during daily work or exercise. Patients usually feel soreness or tightness that builds gradually. With proper physiotherapy guidance and rest, recovery is usually straightforward.
Poor Posture (Common in Desk Jobs)
Sitting for long hours with incorrect posture can place continuous stress on certain muscles, especially in the neck, shoulders, and lower back. Many patients don’t notice this until pain becomes persistent. Correcting posture and strengthening key muscles can significantly reduce discomfort.
Sudden Injury or Lifting
Lifting heavy objects incorrectly or making a sudden movement can strain muscles or ligaments. This type of pain often starts immediately and may limit movement. Early assessment helps prevent the injury from becoming a long-term problem.
Lack of Flexibility or Conditioning
When muscles are stiff or weak due to inactivity, they are more prone to injury even during simple activities. Patients often experience tightness and reduced movement. Gradual strengthening and mobility exercises can safely restore function and prevent future issues.
Nerve Problems (Neurological Pain)
These occur due to:
Nerve compression (like slipped disc)
This occurs when a disc in your spine presses on a nearby nerve, often causing pain that travels to the arm or leg. Patients may feel sharp, shooting pain along with tingling or numbness. Early physiotherapy can help relieve pressure and improve movement safely.
Diabetes-related nerve damage
Over time, high blood sugar levels can affect the health of your nerves, especially in the feet and hands. Patients often describe burning, tingling, or reduced sensation. Managing blood sugar along with guided physiotherapy can help control symptoms and prevent progression.
Spinal conditions (cervical/lumbar spondylosis)
Age-related changes in the spine can lead to stiffness and sometimes nerve irritation. Patients may feel neck or back pain along with radiating symptoms into the limbs. Structured physiotherapy helps improve mobility, strength, and daily function.
Trauma affecting nerve pathways
Injuries from accidents or falls can directly or indirectly impact nerve function. This may result in weakness, altered sensation, or difficulty in movement. A thorough assessment is important to guide safe recovery and determine if specialist referral is needed.
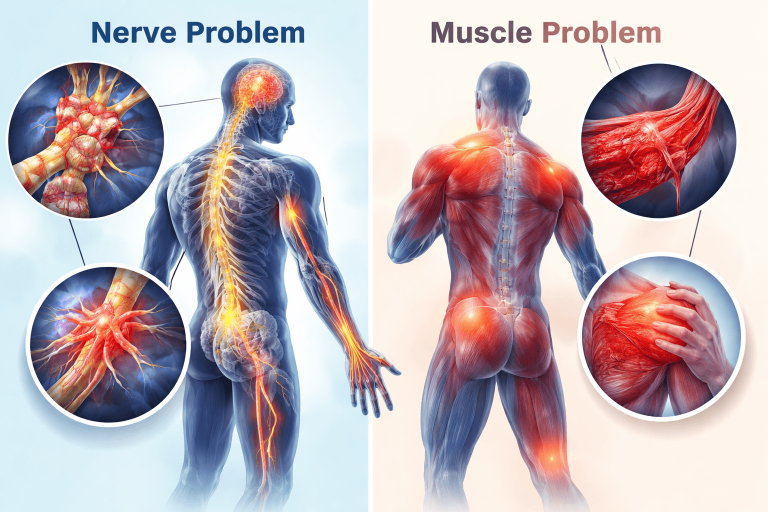
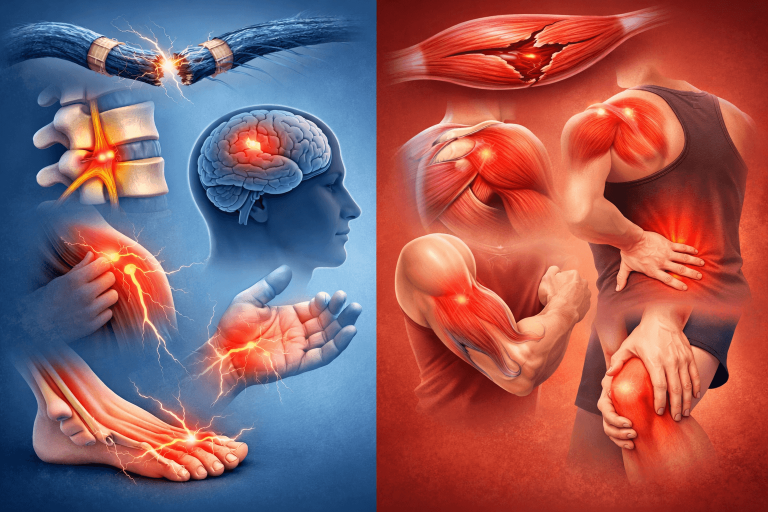
Nerve Problem vs Muscle Problem: Key Differences You Should Know
Understanding your symptoms can offer early clues:
1. Type of Pain
- Muscle pain: Dull, aching, localized
- Nerve pain: Sharp, burning, shooting, electric-like
2. Spread of Pain
- Muscle: Usually stays in one area
- Nerve: Travels along a path (e.g., from back to leg—sciatica)
3. Associated Symptoms
- Muscle: Tightness, stiffness
- Nerve: Tingling, numbness, weakness
4. Response to Movement
- Muscle: Pain increases with movement but improves with rest
- Nerve: Certain movements trigger sharp pain (like bending or coughing)
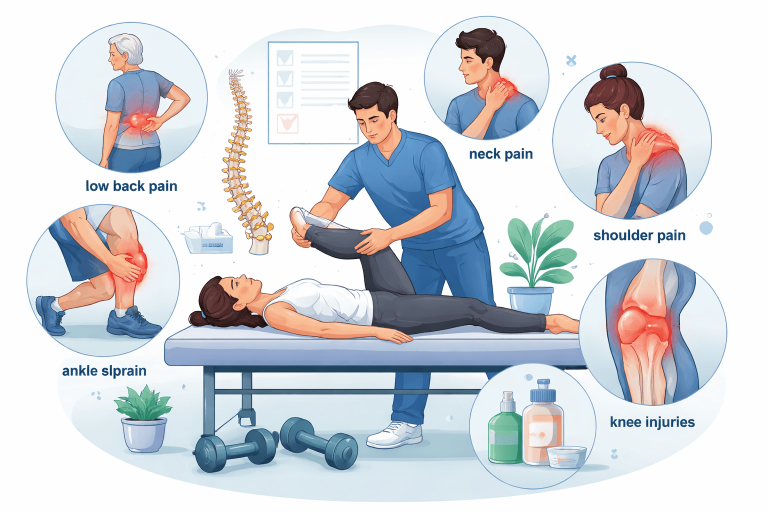
Common Causes Seen at Varia Physiotherapy Clinic
From years of clinical experience, here are patterns we commonly observe:
Muscle-Related Issues
- Office workers with prolonged sitting
- Gym injuries due to improper form
- Sudden lower back strain from lifting
Nerve-Related Issues
- Cervical radiculopathy from long-term mobile use
- Lumbar disc herniation causing leg pain
- Diabetic neuropathy in older adults
According to the World Health Organization, musculoskeletal conditions are among the leading causes of disability worldwide. Similarly, nerve-related disorders significantly impact quality of life if not addressed early.

How Physiotherapy Helps: A Step-by-Step Approach
At Varia Physiotherapy Clinic, treatment is not a one-size-fits-all solution. It begins with clinical reasoning and evidence-based assessment.
Step 1: Detailed Assessment
- Posture analysis
- Range of motion testing
- Neurological screening (reflexes, sensation)
- Functional movement evaluation
This helps us distinguish between nerve and muscle involvement accurately. It ensures that the treatment targets the actual cause of your pain rather than just the symptoms. With a clear diagnosis, recovery becomes more efficient and reduces the risk of the problem returning. It also allows us to guide you with the right exercises and precautions for long-term relief.
Step 2: Diagnosis & Treatment Planning
We create a customized plan based on:
- Severity of symptoms
- Duration of pain
- Patient lifestyle and goals
Step 3: Targeted Treatment
For Muscle Problems
- Manual therapy
- Stretching and strengthening exercises
- Dry needling (if appropriate)
- Postural correction
For Nerve Problems
- Neural mobilization (nerve gliding techniques)
- Spinal decompression exercises
- Pain modulation techniques (IFT, TENS)
- Ergonomic correction
Research from National Institutes of Health supports physiotherapy as a first-line treatment for many musculoskeletal and nerve-related conditions.
Step 4: Education & Prevention
Patients are taught:
- Correct posture
- Home exercise routines
- Activity modifications

Real Patient Scenario from Our Clinic
A 42-year-old male working in IT visited us with severe lower back pain radiating to his right leg. He had been taking painkillers for weeks, assuming it was a muscle strain—without fully understanding whether your pain is coming from a nerve or a muscle, it’s easy to misjudge the cause. After a detailed assessment, we identified it as lumbar nerve compression (sciatica).
Treatment Approach
Neural mobilization
This technique gently moves and “glides” the nerves to reduce irritation and improve their flexibility. Patients with tingling, numbness, or radiating pain often benefit from it. It is done carefully under guidance to avoid aggravating symptoms.
Core stabilization exercises
These exercises strengthen the muscles around your abdomen and lower back, which support your spine. Patients often notice better balance, reduced pain, and improved daily function. Progression is gradual to ensure safety and long-term results.
Postural correction
This focuses on improving how you sit, stand, and move during daily activities. Many patients experience pain due to long-standing poor habits without realizing it. Small, consistent changes in posture can significantly reduce strain and prevent recurring issues.
Outcome
Within 4–6 weeks, his pain reduced significantly, and he returned to work without medication. In contrast, another patient—a 50-year-old homemaker—came with shoulder pain. She feared nerve damage, but it turned out to be a rotator cuff muscle strain, which improved in just 2–3 weeks with physiotherapy.
Myths vs Facts
Myth 1: All pain is due to muscle strain
Fact: Nerve involvement is common, especially with radiating pain
Myth 2: Rest is the best treatment
Fact: Guided movement is often more effective
Myth 3: Painkillers solve the problem
Fact: They only mask symptoms, not the cause
Myth 4: Surgery is always needed for nerve pain
Fact: Most cases improve with conservative physiotherapy
When Should You See a Physiotherapist?
Don’t wait too long if you experience:
- Pain lasting more than 7–10 days
- Tingling or numbness
- Weakness in arms or legs
- Difficulty in daily activities
- Pain that spreads or worsens
When Referral May Be Needed
We may refer you to an orthopedic specialist or neurologist if:
- There is severe nerve compression
- Symptoms worsen despite therapy
- There are signs of serious neurological deficits
Conclusion
Understanding the nerve problem vs muscle problem: key differences you should know empowers you to take the right steps toward recovery. Pain is not just something to tolerate—it’s something to understand.
At Varia Physiotherapy Clinic, we focus on:
- Accurate diagnosis
- Evidence-based treatment
- Patient-centered care
Recovery is a journey, not an instant fix. But with the right guidance, it is absolutely achievable.
Ethical Call-to-Action
If you’re unsure whether your symptoms need attention, it’s okay to start with a simple consultation. Understanding your condition is the first step toward recovery—no pressure, just guidance.
If you’d like to speak with a physiotherapist or book an assessment at Varia Physiotherapy Clinic, you can reach out here:



Our team is here to listen, assess, and guide you toward safe and effective recovery.
Nerve Problem vs Muscle Problem- FAQs
Q1. How do I know if my pain is nerve or muscle-related?
Q2.Can physiotherapy cure nerve pain completely?
Q3. How long does recovery take?
Q4. Is exercise safe during pain?
Q5. Do I need an MRI before physiotherapy?
About the Author

Dr. Hetal M Varia
After a rich experience of working in US healthcare as manager and licensed physiotherapist in US for last 11 years, she has returned home with a vision to become pioneer of Vestibular Therapy and specialized Parkinson physiotherapy in Ahmedabad. With her special skills and expertise in vertigo, Parkinson, balance and movement disorders therapy, Dr. Varia is committed to provide US standards of therapy services , compassionate and patient centered care to our people and community. With a vision of the world where everyone walks strong & steady, she intends to empower individuals with vestibular and neurological disorders through specialized care, rehabilitation & innovative therapies to improve mobility, balance & overall quality of life!