Modern Cervical Spondylosis Treatment In Ahmedabad with Evidence-Based Spine Care
A 42-year-old IT professional from Prahladnagar walked into my clinic holding his MRI report.
“Doctor, it says disc bulge. My fingers are tingling. Is this permanent? Will I need surgery?”
He had:
- Neck pain for 6 months
- Tingling into the right arm
- Tried YouTube traction exercises
- Used muscle relaxants for months
- Compared his recovery with a colleague who “got fine in 10 days”
In my clinical practice in Ahmedabad, the biggest mistake I see in cervical spondylosis patients is treating the MRI report instead of treating the movement problem.
Most online articles fail because they are:
- Too general
- Too exercise-heavy
- No explanation of nerve sensitivity
- No flare management guidance
- No clarity on when to stop
- No ergonomic context (long screen time, mobile posture, two-wheeler commute strain)
This guide is about clarity — not panic.
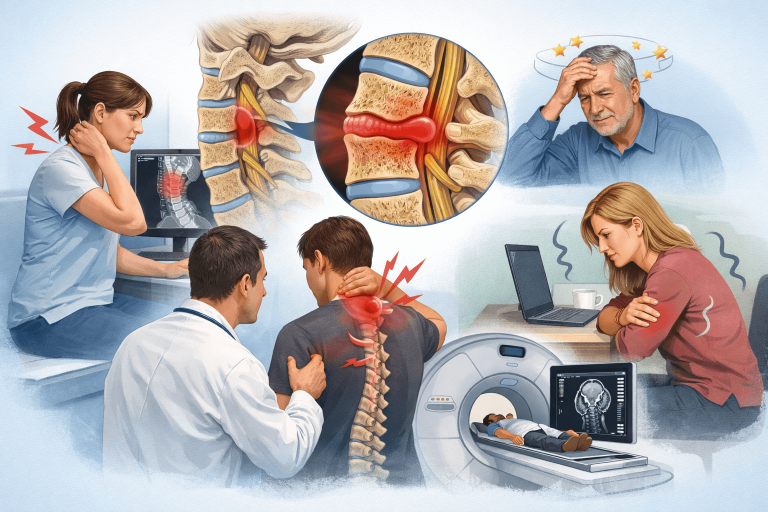
REAL PATIENT PROBLEMS I SEE IN CLINIC
Why Does Neck Pain Keep Returning?
Because the root issue is often:
Poor load tolerance
Your neck tissues may have lost their ability to handle daily stress (long screen time, driving, lifting), so even normal activities trigger pain until strength and endurance are rebuilt gradually.
Weak deep neck stabilizers
When the small support muscles in the front of your neck are underactive, larger muscles overwork, leading to stiffness, fatigue, and recurring pain despite stretching.
Scapular muscle imbalance
If shoulder blade muscles are weak or poorly coordinated, the neck compensates, increasing strain during desk work, mobile use, or overhead activity.
Stress-related muscle guarding
Emotional stress can cause unconscious neck muscle tightening, keeping pain cycles active even when structural damage is minimal.
Why Does Tingling Persist Despite Exercise?
Because nerve tissue is sensitive. It needs graded exposure — not aggressive stretching or forceful traction. Many patients unknowingly irritate the nerve while trying to “fix” it.
The Overuse of Scans
- MRI often shows disc bulges even in people without pain.
- Scan findings ≠ severity of symptoms.
- Fear based on imaging increases muscle tension and slows recovery.
Common Mistakes in Ahmedabad Clinics
- Months of passive modalities only
- No progressive strength plan
- Ignoring workstation setup
- Overstretching instead of stabilizing
- Avoiding all neck movement
- Expecting 7-day recovery
Cervical spondylosis is not an emergency in most cases — but mismanagement makes it chronic, which is why specialized physiotherapy services in Ahmedabad are important for proper and timely care.

STEP-BY-STEP CLINICAL ACTION PLAN
Step 1: Proper Diagnosis & Red Flag Screening
Differentiate:
- Mechanical neck pain
- Nerve root irritation
- Myelopathy (rare but serious)
Red flags:
- Progressive arm weakness
- Loss of bladder/bowel control
- Severe trauma history
- Unexplained weight loss
Step 2: Pain Control Without Over-Reliance on Passive Therapy
What to do:
- Gentle movement
- Isometric activation
- Activity pacing
Why it works:
Movement improves circulation and reduces nervous system hypersensitivity.
Common mistake:
Complete rest or overuse of electrotherapy.
Step 3: Mobility Restoration (Without Aggressive Manipulation)
Goal:
Restore safe, controlled range.
Avoid:
High-velocity manipulations during acute nerve irritation.
Why:
Inflamed nerve roots do not respond well to force.
Step 4: Strength & Load Tolerance Development
Focus on:
Deep neck flexors
These small stabilizing muscles support your cervical spine during sitting, driving, and screen work. In chronic neck pain and cervical spondylosis, they often become weak or poorly coordinated, increasing strain on discs and joints — retraining them improves control, not just posture.
Scapular stabilizers
Muscles around your shoulder blades help offload the neck during arm use and desk work. When they’re weak or overpowered by upper trapezius tension, neck compression increases — restoring balanced control reduces recurring pain and nerve irritation.
Postural endurance
This is your ability to maintain comfortable alignment over time without muscle fatigue or guarding. It’s not about sitting “perfectly straight,” but about building tolerance so daily activities like laptop work or commuting don’t repeatedly flare your symptoms.
Why:
Stronger stabilizers reduce excessive disc loading and improve nerve tolerance.
Mistake:
High-rep resistance band pulls without progression logic.
Step 5: Functional Reintegration
Train:
- Desk tolerance
- Driving posture
- Lifting mechanics
- Phone usage modification
Rehab must reflect real-life demands.
Step 6: Long-Term Relapse Prevention
Includes:
Ergonomic correction
This means adjusting your workstation, screen height, chair support, and driving posture so your neck isn’t under constant low-grade strain. Small corrections reduce cumulative disc and joint stress more effectively than relying only on treatment sessions.
Stress management
Chronic stress increases muscle guarding around the neck and shoulders, amplifying pain sensitivity. Simple breathing strategies, movement breaks, and sleep regulation help calm the nervous system and reduce flare frequency.
Weekly strength maintenance
After recovery, neck and upper back strength must be maintained 1–2 times per week. Without ongoing load exposure, deconditioned muscles fatigue quickly and symptoms often return.
Workload pacing
Gradually increasing screen time, driving hours, or gym activity prevents sudden overload. Sustainable recovery comes from controlled progression, not pushing through pain or resting completely for weeks.
REAL CASE EXAMPLES
Case 1: 39-Year-Old Software Engineer
Duration: 8 months
Symptoms: Neck pain + right arm tingling
Failed attempts:
Random traction + rest.
Plan:
Weeks 1–2: Pain control + nerve-friendly mobility
Weeks 3–6: Stabilization strengthening
Weeks 7–10: Work tolerance retraining
Setback:
Flare during project deadline.
Outcome:
Tingling reduced by 70%. Full-day desk tolerance restored.
Limitation:
Avoids long gaming sessions.
Case 2: 46-Year-Old Gym-Goer
Post-acute disc episode.
Goal:
Return to weight training.
Deficits:
Poor scapular control, excessive cervical extension during lifts.
Modification:
Technique correction
Gradual load reintroduction
Improvement:
Returned to 60% training load in 12 weeks.
Limitation:
Avoids heavy overhead lifting during flare periods.

PATIENT REFLECTIONS
Textile trader, 50:
“I thought disc bulge meant surgery. Now I understand strength matters more.”
Homemaker, 45:
“My tingling scared me. Learning flare management reduced my fear.”
College lecturer, 52:
“It wasn’t posture correction alone — it was endurance training.”
CLINICAL CREDIBILITY
Modern spine guidelines recommend:
- Education
- Exercise-based rehabilitation
- Avoiding unnecessary imaging
- Staying active within tolerance
Pain science research shows: nerve irritation improves with graded exposure — not complete avoidance. Evidence supports structured rehab, including cervical spondylosis treatment in Ahmedabad, over passive-only approaches.
WHO THIS GUIDE IS NOT FOR
This guide is NOT for:
- Sudden severe arm weakness
- Loss of bladder/bowel control
- Major trauma
- Progressive neurological deficit
- Suspected infection
- People expecting instant relief
This guide does NOT:
- Replace medical diagnosis
- Provide medication advice
- Guarantee disc reversal
- Replace in-person evaluation
- Boundaries create safety.
IF I WERE TREATING THIS TODAY
I would prioritize:
- Education first
- Fear reduction
- Gradual load progression
I would avoid:
- Aggressive manipulations during acute nerve pain
- Promising quick fixes
- Excessive rest
One mistake I see repeatedly:
Over-focusing on posture instead of building endurance.
One red flag I never ignore:
Progressive arm weakness.
Referral when:
Neurological deficit worsens or conservative management fails.
CONCLUSION
Key insight:
Cervical spondylosis is usually a load management issue — not a surgical emergency.
What to do next:
- Track symptom triggers
- Build neck endurance gradually
- Adjust workstation
- Avoid panic-based decisions
Resources:
- Download Structured Neck Rehab Checklist
- Use Self Neck-Load Assessment Tool
- Reflect on symptom pattern before changing exercises
No pressure. Just clarity.
Cervical Spondylosis Treatment In Ahmedabad - FAQs
Q1. Will my disc bulge go back to normal?
Q2. Is arm tingling dangerous?
Q3.Do I need an MRI before physiotherapy??
Q4. Can physiotherapy help avoid surgery?
Q5.Why is recovery taking longer than expected?
References
About the Author

Dr. Hetal M Varia
After a rich experience of working in US healthcare as manager and licensed physiotherapist in US for last 11 years, she has returned home with a vision to become pioneer of Vestibular Therapy and specialized Parkinson physiotherapy in Ahmedabad. With her special skills and expertise in vertigo, Parkinson, balance and movement disorders therapy, Dr. Varia is committed to provide US standards of therapy services , compassionate and patient centered care to our people and community. With a vision of the world where everyone walks strong & steady, she intends to empower individuals with vestibular and neurological disorders through specialized care, rehabilitation & innovative therapies to improve mobility, balance & overall quality of life!