Proven & Advanced Arthritis Physiotherapy Treatments in Ahmedabad For Lasting Pain Relief
Last week, a 56-year-old woman from Satellite, Ahmedabad told me:
“Doctor, my X-ray says severe knee arthritis. One doctor said surgery. My neighbor says just walk more. YouTube says do squats. I’m confused and scared.”
She had stopped climbing stairs. Avoided temple steps. Sat less on the floor. Took painkillers for 8 months. Tried random strengthening videos that increased swelling.
In my clinical practice in Ahmedabad, the biggest mistake I see in arthritis patients is not weakness — it’s either over-resting or overdoing exercises.
Most online articles fail because they are:
- Too general
- Too exercise-heavy
- No discussion of load management
- No explanation of flare-ups
- No clarity on when to stop
- No context of our local lifestyle (stairs without lifts, floor sitting, uneven roads, winter stiffness)
This guide is not about “5 best exercises.” It is about making safe decisions with arthritis.
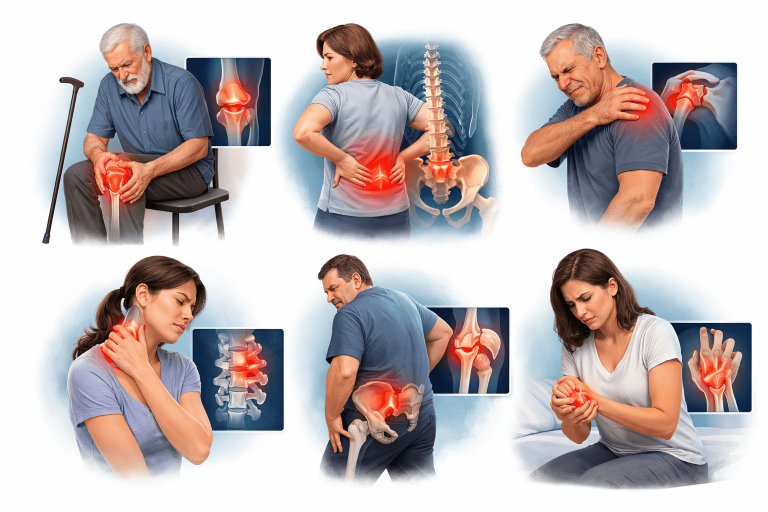
REAL PATIENT PROBLEMS I SEE IN CLINIC
Why Does Arthritis Pain Fluctuate?
Because arthritis is not just “cartilage damage.” It involves:
Synovial inflammation
Inside your joint is a soft lining called the synovium. When it becomes irritated, it produces extra fluid, causing swelling, warmth, and stiffness. In my experience, this is often why your knee feels “tight” in the morning or after overuse not necessarily because damage suddenly worsened.
Muscle weakness
When pain persists, surrounding muscles (like the quadriceps in knee arthritis) naturally reduce their activity. Over time, this weakness increases joint stress during walking and stairs. Many patients think pain causes weakness but weakness also keeps the pain cycle going.
Joint load sensitivity
Arthritic joints become more sensitive to how much force passes through them. This doesn’t mean the joint is fragile — it means its tolerance is reduced. If we increase walking, stairs, and exercises too quickly, the joint reacts with swelling or soreness.
Nervous system sensitization
With long-standing pain, the nervous system can become more alert and protective. This means pain may feel stronger than the actual tissue stress. I often see patients whose scans look moderate, but their pain feels severe — because the pain system has become amplified over time.
Why Did Swelling Increase After Exercise?
Because:
- You increased repetitions too fast
- You added stairs + walking + exercises same day
- You ignored 24-hour pain response
Good exercise does not mean zero discomfort. But it should not cause lasting swelling beyond 24–48 hours.
Misinterpretation of X-rays
- I’ve seen patients with “severe” X-ray changes walking fine.
- And mild X-rays with disabling pain.
- Imaging shows structure.
- It does NOT measure pain tolerance.
- Over-focusing on scan severity delays rehab.
Common Mistakes I See in Ahmedabad
- Only doing passive modalities (IFT, ultrasound) for months
- Ignoring body weight impact
- Wearing worn-out chappals with no support
- Avoiding all movement due to fear
- Comparing recovery with neighbors
- Expecting pain to disappear completely
Arthritis rehab is about capacity building, not pain elimination, with the goal to restore strength and movement naturally over time through consistent and progressive rehabilitation using advanced musculoskeletal physiotherapy treatment.

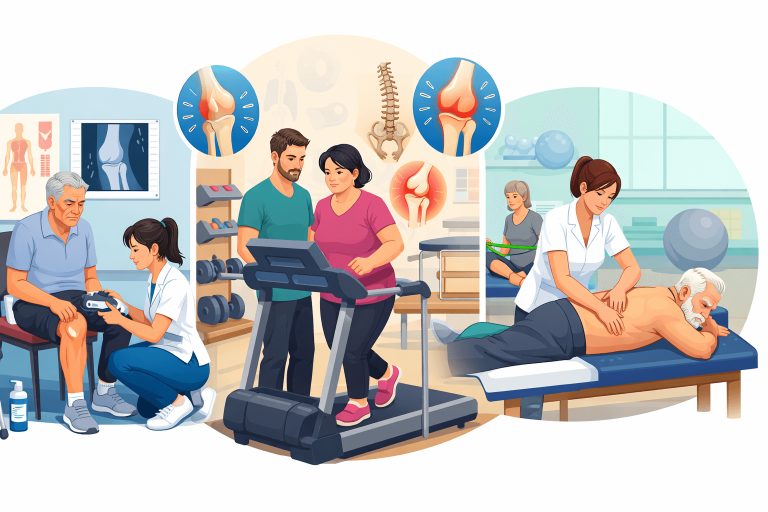
STEP-BY-STEP CLINICAL ACTION PLAN
Step 1: Accurate Diagnosis & Red Flag Screening
Osteoarthritis
Osteoarthritis is a gradual wear-related joint condition, most commonly affecting knees and hips after midlife. It doesn’t mean your joint is “finished” — it means the joint’s load tolerance has reduced. With the right strengthening and activity pacing, many people manage symptoms effectively without rushing toward surgery. For personalized guidance, access expert care for arthritis patients in Ahmedabad to protect your joints and improve daily function.
Rheumatoid arthritis
Rheumatoid arthritis is an autoimmune condition where the body mistakenly attacks the joint lining, causing swelling, warmth, and prolonged morning stiffness. It requires medical treatment from a rheumatologist, and physiotherapy focuses on protecting joints, maintaining mobility, and preventing deformity during flare and non-flare phases.
Post-traumatic arthritis
Post-traumatic arthritis develops after a past injury like a fracture, ligament tear, or joint surgery. Even when the injury heals, altered joint mechanics can lead to early degeneration. Targeted rehabilitation helps restore movement balance and reduce excess stress on the affected joint.
Screen for:
- Sudden severe swelling
- Fever
- Rapid deformity
- Night pain unrelated to movement
Step 2: Pain & Inflammation Control (Without Dependency)
What to do:
- Controlled movement
- Isometric strengthening
- Activity pacing
- Thermal therapy (when appropriate)
Why it works:
Gentle muscle activation improves circulation and reduces joint stress sensitivity.
What patients do wrong:
- Complete rest for weeks
- Overuse painkillers
- Expect machines to fix the problem
Step 3: Restore Safe Joint Mobility
Goal:
Improve joint nutrition and reduce stiffness.
Method:
- Low-load range work
- Assisted mobility
- Avoid forced end-range during flare-ups
Biology:
Movement stimulates synovial fluid distribution.
Common mistake:
Aggressive stretching during inflammation.
Step 4: Strength & Load Tolerance Building
This is the real treatment phase.
Focus on:
Quadriceps strength (knee OA)
The quadriceps muscle (front of your thigh) acts like a natural shock absorber for the knee. When it’s weak, more load goes directly into the joint, increasing pain during stairs or standing up. Strengthening it safely improves knee stability and reduces joint stress — not by “fixing cartilage,” but by improving support. This is why structured Arthritis Physiotherapy Treatments In Ahmedabad often focus heavily on targeted quadriceps strengthening to reduce pain and improve daily function safely.
Gluteal strength (hip arthritis)
Your gluteal muscles control hip alignment when you walk. If they are weak, the hip joint experiences uneven loading, which can worsen pain. Improving glute strength often reduces limping and improves walking tolerance more effectively than stretching alone.
Grip and intrinsic hand muscles (RA cases)
In rheumatoid arthritis, small hand joints can become inflamed and unstable. Strengthening the small intrinsic hand muscles helps protect joint alignment and maintain daily function like opening jars or holding utensils. Exercises must be adjusted during flare-ups to avoid irritation.
Why:
Stronger muscles reduce joint compression stress.
Mistake:
High-rep light exercises without progression.
Step 5: Functional Reintegration
Train:
- Stair tolerance
- Sit-to-stand
- Modified squatting
- Walking progression
Gradual exposure prevents flare cycles.
Step 6: Long-Term Joint Protection
Includes
- Weight management
- Footwear correction
- Weekly strength maintenance
- Flare tracking
Read More: Cost Of Physiotherapy In Ahmedabad
REAL CASE EXAMPLES
Case 1: Sedentary Knee Osteoarthritis
- Age: 58
- Duration: 3 years
- On painkillers 6 months
- Avoiding stairs
Failed attempts:
Random online exercises → swelling increased.
Treatment:
Week 1–2: Pain control + isometrics
Week 3–6: Progressive strengthening
Week 7–10: Stair retraining
Setback:
One flare after the wedding function (overuse).
Outcome:
Climbs 2 floors independently. Still mild discomfort in winter.
Expectation:
Condition managed, not cured.
Case 2: 48-Year-Old Working Professional (Early Hip Arthritis)
Goal:
Return to 3 km daily walking.
Deficits:
Glute weakness, altered gait.
Plan:
Load modification
Strength progression
Step count monitoring
Improvement:
Pain reduced from 7/10 to 3/10 in 8 weeks.
Walk 2.5 km comfortably.
Limitation:
Avoids deep floor sitting.
Maintenance:
2 strength sessions/week.

NATURAL PATIENT REFLECTIONS
School teacher, 62:
“I thought exercise would wear out my knee. Now I understand controlled loading helps.”
Bank employee, 54:
“I was scared of surgery. Now I know when it’s necessary and when it’s not.”
Homemaker, 60:
“My pain didn’t disappear, but I can manage it without fear.”

CLINICAL CREDIBILITY
International guidelines for osteoarthritis recommend:
- Strength training
- Aerobic activity
- Weight management
- Education
The WHO also supports regular moderate physical activity for joint health. Research consistently shows:
Exercise reduces arthritis pain similar to medication in mild-to-moderate cases — without drug side effects.
But exercise must be:
- Progressive
- Measured
- Individualized
WHO THIS GUIDE IS NOT FOR
This guide is NOT for:
- Acute joint infection
- Sudden traumatic swelling
- Suspected fracture
- Rapid deformity
- Progressive neurological weakness
- Severe inflammatory flare
- People expecting instant relief
This guide does NOT:
- Replace medical diagnosis
- Replace rheumatology consultation
- Provide medication advice
- Guarantee cartilage regeneration
- Replace in-person assessment
Boundaries build trust.
IF I WERE TREATING THIS TODAY
I would prioritize:
- Education first
- Fear reduction
- Gradual load exposure
I would avoid:
- Aggressive passive modalities
- Deep squats in early stage
- Promising pain-free outcome
One mistake I repeatedly see:
Patients either stop movement completely or jump into intense workouts.
One red flag I never ignore:
Sudden severe swelling with fever.
Referral when:
- Inflammatory arthritis suspected
- Severe joint collapse
- Failed conservative management after structured trial
CONCLUSION
Key insight:
Arthritis management is about building joint capacity, not eliminating every pain signal.
What you should do next:
- Track flare patterns
- Start structured strength work
- Avoid random exercise changes
- Monitor 24-hour pain response
Educational Resources:
- Download Arthritis Flare Tracker
- Use Joint Load Self-Assessment Checklist
- Reflect on your symptom pattern before changing exercises
No pressure. Just clarity.
Arthritis Physiotherapy Treatments In Ahmedabad - FAQs
Q1. Will my arthritis fully go away?
Q2.Is pain during exercise normal?
Q3. Do I need an MRI?
Q4. Can physiotherapy delay surgery?
Q5.What if physiotherapy fails?
References
About the Author

Dr. Hetal M Varia
After a rich experience of working in US healthcare as manager and licensed physiotherapist in US for last 11 years, she has returned home with a vision to become pioneer of Vestibular Therapy and specialized Parkinson physiotherapy in Ahmedabad. With her special skills and expertise in vertigo, Parkinson, balance and movement disorders therapy, Dr. Varia is committed to provide US standards of therapy services , compassionate and patient centered care to our people and community. With a vision of the world where everyone walks strong & steady, she intends to empower individuals with vestibular and neurological disorders through specialized care, rehabilitation & innovative therapies to improve mobility, balance & overall quality of life!